Washington University Researchers Identify Novel Pathway to Halt Age-Related Macular Degeneration Through Cholesterol Metabolism
Age-related macular degeneration (AMD) remains one of the most formidable challenges in modern ophthalmology, serving as a primary driver of irreversible vision loss for millions of individuals globally. However, a landmark study led by the Washington University School of Medicine in St. Louis has unveiled a promising new therapeutic target that could fundamentally alter the trajectory of the disease. By investigating the intricate relationship between cholesterol metabolism and cellular degradation, researchers have identified a specific molecule, apolipoprotein M (ApoM), as a potential key to slowing or even blocking the progression of this debilitating condition. The findings, published June 24 in the journal Nature Communications, not only offer hope for those suffering from vision loss but also suggest a profound systemic link between ocular health and cardiovascular disease.
The Growing Crisis of Age-Related Macular Degeneration
To understand the significance of the Washington University study, one must first grasp the scale and impact of age-related macular degeneration. As the global population ages, the prevalence of AMD is expected to rise sharply. According to the BrightFocus Foundation, approximately 11 million people in the United States alone currently live with some form of AMD, a number expected to double to 22 million by 2050. Globally, the number of people affected by the disease is projected to reach 288 million by 2040.
AMD primarily targets the macula, the central part of the retina responsible for sharp, detailed vision. When the macula deteriorates, individuals lose the ability to perform essential daily tasks such as reading, driving, and recognizing faces. The disease typically manifests in two forms: "dry" and "wet." Dry AMD, which accounts for about 80% to 90% of cases, involves the gradual thinning of the macula and the accumulation of yellow deposits called drusen. These deposits are rich in cholesterol and proteins. As drusen grow, they trigger chronic inflammation and cellular damage, leading to geographic atrophy—a form of advanced neurodegeneration that mirrors the cellular death seen in Alzheimer’s disease. Wet AMD, though less common, is more aggressive and occurs when abnormal blood vessels grow underneath the retina, leaking fluid and blood that cause rapid vision loss.
The Role of Cholesterol Metabolism in Ocular Decay
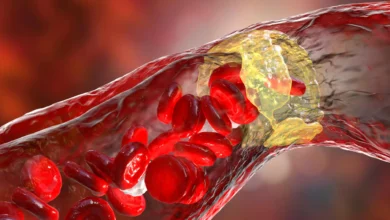
For years, clinicians have noted a statistical correlation between cardiovascular health and the risk of macular degeneration. Both conditions share common risk factors, including age, smoking, and high blood pressure. The new research from WashU Medicine provides a biological explanation for this correlation: dysfunctional cholesterol metabolism.
Dr. Rajendra S. Apte, the Paul A. Cibis Distinguished Professor of Ophthalmology and Visual Sciences and the study’s senior author, explains that during routine eye exams, doctors often observe cholesterol-rich drusen under the retina. In the early stages of the disease, patients may not notice any changes in their vision, but the presence of these lipids signals a breakdown in the body’s ability to clear cellular waste.
The study posits that the accumulation of these lipids is not merely a byproduct of aging but a result of a failure in the "good cholesterol" pathways. When cells in the retina cannot efficiently process and remove cholesterol, it triggers a cascade of inflammation and oxidative stress that eventually destroys light-sensing cells. This metabolic failure is not localized to the eye; it is a systemic issue that also affects the heart.
Apolipoprotein M: The Body’s Natural Cleanup Crew
The crux of the research lies in the discovery of the protective role of apolipoprotein M (ApoM). ApoM is a molecule found in the blood that is closely associated with high-density lipoprotein (HDL), commonly known as "good cholesterol." Previous studies have suggested that ApoM possesses anti-inflammatory properties and plays a vital role in maintaining vascular health.
Dr. Apte and his co-senior author, Dr. Ali Javaheri, an assistant professor of medicine and a cardiologist at WashU, hypothesized that declining levels of ApoM might be the common denominator in both AMD and heart failure. Their investigation confirmed that patients with macular degeneration exhibited significantly lower levels of circulating ApoM compared to healthy individuals of the same age. This mirrored earlier findings by Dr. Javaheri, which showed that patients with various forms of heart failure also suffered from an ApoM deficiency.
The research team discovered that ApoM acts as a critical component in the pathways that "mop up" excess cholesterol from tissues. By facilitating the transport of these lipids to the liver for disposal, ApoM prevents the buildup of toxic deposits. Furthermore, the study revealed that ApoM must bind to a signaling molecule called sphingosine-1-phosphate (S1P) to exert its protective effects. Together, this complex triggers a signaling pathway within cells that activates lysosomes—the cell’s "garbage disposal" units—to break down and eliminate cholesterol.
Experimental Success and the Reversal of Damage
To test the therapeutic potential of ApoM, the researchers utilized mouse models of macular degeneration. They employed two primary methods to increase ApoM levels: genetic modification and plasma transfer from healthy mice.
The results were striking. Mice with elevated ApoM levels showed marked improvements in retinal health. The researchers observed a significant reduction in the accumulation of cholesterol deposits and, more importantly, a restoration of function in the light-sensing cells of the retina. This suggests that increasing ApoM does not just stop new damage from occurring but helps the eye recover some of its metabolic efficiency.
"Our findings suggest that developing treatments that increase ApoM levels could treat or even prevent the disease and therefore preserve people’s vision as they age," Dr. Apte stated. This is a significant departure from current treatments, such as anti-VEGF injections, which are primarily used to manage the "wet" form of the disease by slowing abnormal blood vessel growth. While these treatments are effective at preventing further vision loss in advanced stages, they do not address the underlying metabolic causes of the disease and cannot reverse existing damage.
A Shared Vulnerability: The Heart and the Eye
One of the most profound implications of this study is the realization that retinal pigment epithelial cells and heart muscle cells share a similar vulnerability to low ApoM levels. Both types of cells are highly metabolic and require efficient waste-disposal systems to function correctly over several decades.
"It is possible that the interaction between ApoM and S1P is regulating cholesterol metabolism in both cell types," Dr. Javaheri noted. This insight opens the door for a unified approach to treating diseases of aging. A therapy designed to boost ApoM levels could potentially serve as a dual-purpose treatment, protecting the vision of elderly patients while simultaneously strengthening their cardiovascular systems against heart failure.
This systemic perspective is crucial given the economic and social burden of these diseases. In the United States, heart failure affects approximately 6.2 million adults and is a leading cause of hospitalization. By addressing the metabolic roots of these conditions, researchers hope to reduce the overall burden on the healthcare system and improve the quality of life for the aging population.
From Research to Reality: The Path Toward New Therapies
The transition from laboratory discovery to clinical application is already underway. Dr. Apte and Dr. Javaheri, in collaboration with Washington University’s Office of Technology Management (OTM), have launched a startup company called Mobius Scientific. Founded in 2022, Mobius Scientific aims to harness the research findings to develop novel pharmacological interventions that can elevate ApoM levels in patients.
The path to a viable drug involves several challenges, including determining the most effective delivery method—whether through oral medication, periodic injections, or gene therapy—and ensuring that the treatment maintains the necessary ApoM-S1P balance. However, the foundational data provided by the Nature Communications study provides a clear roadmap for drug development.
Analysis of Implications: A Paradigm Shift in Geriatric Medicine
The Washington University study represents a paradigm shift in how we view age-related diseases. Rather than treating the eye and the heart as isolated systems, this research encourages a more holistic, metabolic-focused approach to geriatric medicine.
If ApoM-based therapies prove successful in human clinical trials, they could offer the first preventative treatment for dry AMD. Currently, patients diagnosed with early-stage dry AMD are often told there is little that can be done beyond taking vitamin supplements (such as the AREDS2 formula) and monitoring their vision. The ability to intervene early by restoring cholesterol metabolism could save the sight of millions who would otherwise progress toward geographic atrophy.
Furthermore, the study highlights the importance of interdisciplinary collaboration. By combining the expertise of an ophthalmologist and a cardiologist, the research team was able to identify a biological mechanism that might have remained hidden if they had focused on only one organ system. This "cross-talk" between specialties is increasingly seen as the future of medical innovation.
As the scientific community continues to analyze these findings, the focus will shift toward long-term safety and efficacy in humans. The support from the National Institutes of Health (NIH) and various private foundations underscores the high priority placed on finding a solution to AMD. For now, the discovery of ApoM’s role provides a vital new chapter in the fight against blindness and age-related decline, offering a vision of a future where aging does not inevitably lead to the loss of sight or heart function.