Artificial Light at Night Linked to Increased Brain Stress and Elevated Cardiovascular Risk According to New Research

A groundbreaking preliminary analysis set to be presented at the American Heart Association’s Scientific Sessions 2025 has identified a significant correlation between exposure to artificial light at night and a heightened risk of cardiovascular disease. The study, which utilizes advanced neuroimaging and satellite data, suggests that light pollution acts as a potent environmental stressor, triggering a biological cascade that includes increased brain stress signals and systemic arterial inflammation. As urban environments become increasingly saturated with artificial illumination, researchers are warning that "nightglow" may be a neglected but critical factor in the global rise of heart-related ailments.
The research will be a focal point of the upcoming Scientific Sessions, scheduled to take place from November 7 to 10 in New Orleans. This annual gathering is a premier venue for the disclosure of high-impact cardiovascular science, attracting thousands of clinicians and researchers from across the globe. The findings presented by the investigative team provide the first concrete evidence of a specific biological pathway connecting the brightness of a person’s nocturnal environment to the physical health of their heart and blood vessels.
The Biological Pathway of Light-Induced Stress
The core of the study revolves around the discovery of a nearly linear relationship between nighttime light exposure and the development of heart disease. According to lead author Shady Abohashem, M.D., M.P.H., head of cardiac PET/CT imaging trials at Massachusetts General Hospital and an instructor at Harvard Medical School, the mechanism is rooted in the brain’s response to environmental stimuli. When the human body is exposed to artificial light during hours traditionally reserved for darkness, the brain perceives this as a stressor.
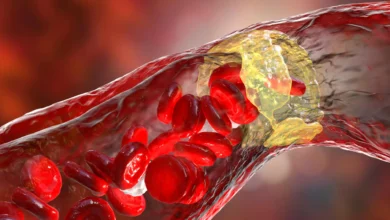
This perception of stress is not merely psychological; it manifests physically through the activation of specific neural pathways. When the brain’s stress centers are triggered by light, they send signals to the rest of the body that can initiate an immune response. This response leads to inflammation within the blood vessels. Over a prolonged period, chronic inflammation results in the hardening of the arteries—a condition known as atherosclerosis—which is the primary precursor to catastrophic events such as myocardial infarctions (heart attacks) and strokes.
The investigators highlighted that while the medical community has long recognized the dangers of air and noise pollution, light pollution has remained largely unstudied in the context of cardiovascular pathology. The modern urban setting, characterized by ubiquitous streetlights, neon signage, and residential "light trespass," means that millions of people are living in a state of perpetual physiological alertness, even while attempting to rest.
Methodology: Combining Satellite Data with Advanced Neuroimaging
To reach these conclusions, the research team conducted a sophisticated analysis involving 450 adult participants. A defining feature of the study was its stringent selection criteria: all subjects were free of pre-existing heart disease and active cancer at the time of the study, allowing researchers to observe the early markers of cardiovascular risk without the confounding variables of established illness.
The study employed a dual-imaging approach using combined Positron Emission Tomography (PET) and Computed Tomography (CT) scans. This technology is uniquely suited for this type of research because it allows for the simultaneous assessment of different bodily functions. The CT portion of the scan provides a highly detailed anatomical map of the body, while the PET portion reveals metabolic and functional activity within tissues.
By using this "one-stop-shop" imaging technique, Dr. Abohashem and his team were able to measure two critical metrics in a single session:
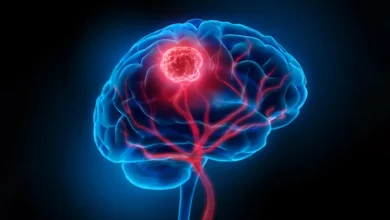
- Brain Stress Activity: Specifically looking at the metabolic activity in the amygdala and other regions associated with the body’s "fight or flight" response.
- Arterial Inflammation: Measuring the level of metabolic activity in the walls of the arteries, which serves as a proxy for inflammation and early-stage plaque buildup.
These clinical measurements were then cross-referenced with high-resolution satellite data from the Visible Infrared Imaging Radiometer Suite (VIIRS). This satellite imagery allowed the researchers to quantify the exact level of outdoor artificial light at the residential addresses of the participants. By merging geographic data with clinical neuroimaging, the study created a comprehensive profile of how a person’s external environment dictates their internal physiological state.
Chronology of Scientific Context and Recent Guidance
The presentation of this study comes at a pivotal moment in the field of circadian medicine. Just weeks prior to the scheduled conference, on October 28, 2024, the American Heart Association issued a formal scientific statement titled "The Role of Circadian Health in Cardiometabolic Health and Disease Risk." This statement served as a foundational document, asserting that the disruption of the body’s internal clocks—the circadian rhythms—is a major contributor to metabolic syndrome, obesity, and cardiovascular issues.
The timeline of these developments reflects an accelerating interest in how the 24-hour cycle of light and dark regulates human health. The October statement noted that even low levels of light pollution can suppress the production of melatonin, the hormone responsible for signaling sleep to the body. Melatonin suppression delays sleep onset and degrades sleep quality, both of which are linked to hypertension and insulin resistance.
The new research by Dr. Abohashem’s team builds upon this foundation by identifying the "how." While the AHA statement focused on the broader implications of circadian disruption, the current study pinpointed the brain-to-artery stress pathway as a primary driver of the damage. This chronological progression from identifying a general risk (circadian disruption) to mapping a specific biological mechanism (brain stress and arterial inflammation) marks a significant leap in cardiovascular science.
Supporting Data and Statistical Trends
The findings of the study suggest that the risk associated with light pollution is dose-dependent. The data indicated that as the intensity of nighttime light increased, there was a proportional increase in the metabolic activity of the brain’s stress centers. Even participants living in areas with what might be considered "modest" levels of light pollution showed measurable increases in arterial inflammation compared to those living in truly dark environments.
This trend is particularly concerning given the global trajectory of urbanization. Estimates suggest that more than 80% of the world’s population lives under "light-polluted" skies, and in the United States and Europe, that figure exceeds 99%. The "linear relationship" found in the study suggests that there may be no safe threshold for artificial light at night; rather, every increment of light contributes to an incremental increase in cardiovascular risk.
Furthermore, the study’s longitudinal follow-up for heart events allowed researchers to see how these early markers of inflammation translated into actual clinical outcomes. Over the observation period, those with higher baseline light exposure and higher initial brain stress levels were significantly more likely to experience major adverse cardiovascular events (MACE).
Expert Reactions and Public Health Implications
The novelty of the research has drawn attention from leading figures in sleep and cardiovascular medicine. Julio Fernandez-Mendoza, Ph.D., a professor at Pennsylvania State University and a member of the AHA writing committee on sleep health, emphasized the public health urgency of these findings. Although not directly involved in the study, Fernandez-Mendoza noted that the research confirms a long-held suspicion: that the brain’s response to the environment is a primary mediator of heart health.
"We have known for some time that excessive light at night is detrimental, but the ‘missing link’ has been the specific pathway of harm," Fernandez-Mendoza stated. "By investigating the stress response of the brain, this study provides a clear target for both clinical intervention and public policy."
The implications for public policy are substantial. If light pollution is viewed through the same lens as air or water pollution, it necessitates a shift in how cities are designed and managed. Potential interventions discussed by the researchers and supporting experts include:
- Urban Lighting Reform: Implementing "dark sky" policies that require streetlamps to be shielded so that light is directed downward toward the ground rather than upward or outward into windows.
- Spectral Adjustments: Moving away from blue-rich LED lighting, which is known to be particularly disruptive to circadian rhythms, toward warmer tones.
- Motion-Sensing Technology: Utilizing smart street lighting that only illuminates when pedestrians or vehicles are present, thereby reducing the total duration of light exposure for nearby residents.
On a personal level, the study suggests that individuals can take immediate steps to mitigate their risk. Recommendations include using blackout curtains, removing electronic devices from the bedroom, and avoiding the "blue light" emitted by smartphones and televisions in the hour preceding sleep.
Limitations and Future Research Directions
While the study is being hailed as a major step forward, the authors were careful to note its limitations. As an observational study based on previously collected data, it can identify correlations but cannot definitively prove a cause-and-effect relationship. There is always the possibility that other factors common to bright urban areas—such as higher levels of noise or sedentary lifestyles—could contribute to the observed risks.
Additionally, the study population was drawn from a single hospital system. While this provided a consistent environment for the PET/CT scans, it means the results may not be fully representative of more diverse populations with different socioeconomic or genetic backgrounds.
Dr. Abohashem expressed a desire to expand the research into larger, multi-center trials. Future studies will likely focus on whether specific interventions—such as the use of blue-light-blocking glasses or the installation of blackout shades—can measurably reduce the brain stress signals and arterial inflammation identified in this preliminary work.
Conclusion: A New Era of Environmental Cardiology
The research to be presented at the American Heart Association’s Scientific Sessions 2025 marks a turning point in our understanding of environmental health. It suggests that the "great transition" to an electrified, 24-hour society has come with a hidden physiological cost. By demonstrating that light pollution is more than a mere aesthetic "annoyance" and is instead a driver of systemic inflammation and brain stress, the study elevates light pollution to the status of a major public health concern.
As clinicians and policymakers gather in New Orleans this November, the findings will likely spark a broader conversation about the "right to darkness." In the quest to prevent heart disease—the leading cause of death globally—the solution may involve not just new medications or surgical techniques, but a fundamental return to the natural cycles of light and dark that have governed human physiology for millennia. The study serves as a potent reminder that the environment we build for ourselves has a profound and measurable impact on the very rhythm of our hearts.