AI spots deadly heart risk most doctors can’t see
A groundbreaking study led by researchers at Johns Hopkins University has unveiled a new artificial intelligence model capable of predicting sudden cardiac death with significantly higher accuracy than current clinical standards. The system, known as Multimodal AI for ventricular Arrhythmia Risk Stratification, or MAARS, leverages deep learning to analyze complex heart imaging and comprehensive medical records, identifying subtle patterns that indicate a high risk of fatal arrhythmias. This technological leap addresses a critical gap in cardiology, where traditional diagnostic methods have long struggled to distinguish between patients who require life-saving interventions and those who can safely avoid them.
The research, funded by federal grants and published in the journal Nature Cardiovascular Research, represents a major milestone in precision medicine. By integrating long-underused data from cardiac imaging with a patient’s full clinical history, the MAARS model provides a granular survival assessment that could prevent thousands of premature deaths while simultaneously sparing patients from the physical and psychological burdens of unnecessary medical procedures.
The Challenge of Hypertrophic Cardiomyopathy
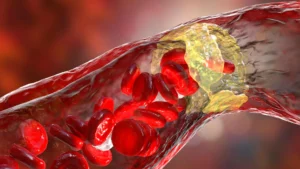
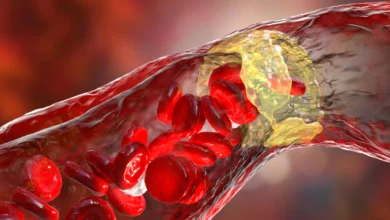
Hypertrophic cardiomyopathy (HCM) is a complex and often inherited heart condition characterized by the abnormal thickening of the heart muscle, particularly the left ventricle. This thickening can make it harder for the heart to pump blood and, more dangerously, can disrupt the heart’s electrical system, leading to life-threatening heart rhythms known as ventricular arrhythmias.
Statistically, HCM is the most common genetic heart disease, affecting between one in 200 and one in 500 individuals globally. Despite its prevalence, the disease is notoriously difficult to manage because its progression varies wildly between patients. While many individuals with HCM live full, asymptomatic lives, the condition remains a leading cause of sudden cardiac death in young people and competitive athletes. For decades, the medical community has sought a reliable "red flag" to identify which patients are at risk of dropping dead without warning, but the complexity of the heart’s geometry and the nuances of tissue scarring have made this an elusive goal.
The "Dice Throw" of Current Clinical Guidelines
Currently, cardiologists in the United States and Europe rely on standardized clinical guidelines to determine which HCM patients should receive an Implantable Cardioverter Defibrillator (ICD). An ICD is a small, battery-powered device placed in the chest that monitors heart rhythms and delivers an electric shock if it detects a dangerous arrhythmia. While life-saving, the implantation of an ICD is an invasive surgery that carries risks of infection, lead failure, and "inappropriate shocks," which can be traumatic for the patient.
The senior author of the study, Natalia Trayanova, a professor of biomedical engineering and medicine at Johns Hopkins, points out that the current risk-stratification tools are woefully inadequate. "Currently, we have patients dying in the prime of their life because they aren’t protected, and others who are putting up with defibrillators for the rest of their lives with no benefit," Trayanova stated. She noted that existing guidelines are accurate only about 50% of the time—a statistic she likens to "throwing dice."
These traditional models often rely on high-level metrics such as the maximum thickness of the heart wall or family history. However, these metrics do not account for the microscopic structural changes within the heart tissue, specifically the distribution of fibrosis, or scarring, which acts as the primary substrate for lethal arrhythmias.
How MAARS Deciphers Hidden Cardiac Data
The MAARS model represents a shift from generalized medicine to personalized data science. The "multimodal" aspect of the AI refers to its ability to synthesize different types of data: patient demographics, clinical history, and, most importantly, contrast-enhanced Magnetic Resonance Imaging (MRI).
In patients with HCM, the heart muscle often develops areas of fibrosis. On a cardiac MRI, these areas are highlighted using a contrast agent called gadolinium. While radiologists can see large areas of scarring, the human eye is incapable of processing the intricate, pixel-level patterns of how that scar tissue is distributed and how it interacts with healthy muscle.
"People have not used deep learning on those images in this way before," Trayanova explained. "We are able to extract this hidden information in the images that is not usually accounted for." The AI model uses deep learning algorithms—specifically neural networks designed for image recognition—to scan the MRI scans. It identifies specific "arrhythmogenic" signatures—structural arrangements of scar tissue that are most likely to trigger a fatal electrical short-circuit in the heart.
By combining these imaging insights with a decade’s worth of clinical data, MAARS builds a comprehensive risk profile for every individual, moving beyond the "one-size-fits-all" approach of current cardiology.
Comparative Success and Statistical Validation
To validate the model, the research team conducted a rigorous retrospective study using data from real patients treated at Johns Hopkins Hospital and the Sanger Heart & Vascular Institute in North Carolina. The cohort included a diverse range of patients with varying degrees of disease progression.
The results were stark. While traditional clinical guidelines hovered at a 50% accuracy rate, the MAARS model achieved an overall accuracy of 89%. Even more impressive was the model’s performance in the most vulnerable demographic: patients aged 40 to 60. In this group, which represents the population at the highest risk for sudden cardiac death in the context of HCM, the AI’s predictive accuracy rose to 93%.
Beyond just a "yes or no" prediction, the AI also provides an "explainability" component. It can describe the specific features in the heart’s geometry or scarring pattern that led to its high-risk classification. This allows cardiologists to understand the "why" behind the AI’s recommendation, fostering a collaborative environment where technology assists rather than replaces human clinical judgment.
Implications for Patient Care and Healthcare Economics
The potential impact of this technology on the healthcare system is twofold: saving lives and reducing medical waste.
For high-risk patients who were previously overlooked by standard guidelines, the MAARS model acts as a literal lifesaver. Identifying these "silent" risks allows for the timely implantation of ICDs, preventing sudden deaths in young and middle-aged adults who would otherwise have no indication of their impending cardiac arrest.
Conversely, for the large number of patients currently living with "unnecessary" ICDs, the model offers a path toward a higher quality of life. ICDs require regular maintenance, battery replacements every few years, and carry a lifelong risk of complications. If a patient is identified by AI as being at extremely low risk, they may be spared the surgery and the subsequent anxiety of living with an implanted device.
"Our study demonstrates that the AI model significantly enhances our ability to predict those at highest risk compared to our current algorithms and thus has the power to transform clinical care," said co-author Jonathan Crispin, a cardiologist at Johns Hopkins. From a healthcare economics perspective, reducing the number of unnecessary ICD implantations could save the insurance and hospital systems millions of dollars annually, as the cost of the device and the procedure often exceeds $30,000 to $50,000 per patient, not including long-term follow-up care.
A Growing Portfolio of AI in Cardiology
This is not the first time Natalia Trayanova’s lab has made waves in the field of computational cardiology. In 2022, her team developed a similar multimodal AI model designed for patients who had suffered previous heart attacks (infarcts). That model focused on predicting the timing of potential cardiac arrests based on the specific location of dead heart tissue.
The success of the MAARS model builds on that foundation, applying the logic of deep learning to the more complex, diffuse scarring found in HCM. The consistent success of these models suggests that the future of cardiology lies in "digital twins"—computational models of a patient’s heart that can be tested and analyzed in a virtual environment before any physical intervention occurs.
Future Directions and Expansion
The Johns Hopkins team is not stopping with hypertrophic cardiomyopathy. Plans are already underway to expand the MAARS algorithm to other types of heart diseases that involve scarring and arrhythmia risk. This includes cardiac sarcoidosis—an inflammatory disease that can cause clumps of abnormal cells to form in the heart—and arrhythmogenic right ventricular cardiomyopathy (ARVC), another leading cause of sudden death in athletes.
Furthermore, the researchers intend to conduct prospective clinical trials. While the retrospective data is compelling, the next step involves using the AI in real-time clinical settings to guide treatment decisions and observing the long-term outcomes of those patients.
As the team refines the algorithm, they are also looking at ways to integrate other data streams, such as genetic sequencing and wearable device data (like heart rate variability from smartwatches), to create an even more dynamic risk assessment tool.
Conclusion
The development of the MAARS model marks a turning point in the fight against sudden cardiac death. By turning to the "hidden" data within MRI images that has been overlooked for years, researchers have provided a solution to a problem that has baffled cardiologists for decades. As this technology moves toward clinical implementation, it promises a future where heart disease is no longer a game of chance, but a condition managed with the precision of advanced mathematics and deep learning. For the millions of people living with hypertrophic cardiomyopathy, the MAARS model offers more than just a data point; it offers the clarity and security of knowing their true risk, potentially saving their lives in the process.