Heather McMahan Shares Her Journey Navigating Eczema: Understanding the Varied Landscape of Atopic Dermatitis

For comedian and podcaster Heather McMahan, eczema has never been a predictable condition. Flare-ups can emerge without warning, often at the most inconvenient times and in visible locations, presenting a significant challenge for someone in the public eye. McMahan’s experience is far from unique; atopic dermatitis (AD), the most common form of eczema, affects millions in the United States. While many recognize AD by its hallmark symptoms—rashes, inflammation, dry, flaky skin, and intense itching—the condition’s presentation can vary significantly from person to person and evolve over time. Despite its prevalence, the exact causes of AD remain a subject of ongoing research, with current understanding pointing to a complex interplay between genetics and environmental triggers, as noted by the National Eczema Association. This inherent variability is precisely what makes managing eczema so challenging, a reality that McMahan has candidly discussed.
The Evolving Landscape of Adult Eczema
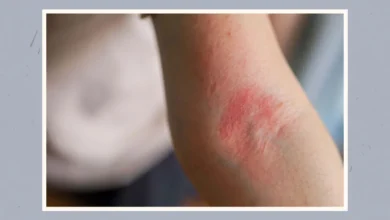
McMahan’s journey with eczema has been a lifelong one, marked by shifts in how the condition manifests. A significant observation for her has been the difference in flare-up locations between childhood and adulthood. While eczema often appears on the cheeks, scalp, and trunk in infants and young children, the American Academy of Dermatology and Mayo Clinic indicate that adult flare-ups are more commonly found on the neck, the inner elbows, behind the knees, and specific facial areas.
"Being in the spotlight, there’s always pressure to look your best, but eczema doesn’t care if you are about to walk on stage or be on television," McMahan shared. "There have been times before a show when a flare popped up on my face or neck, and I just had to roll with it." She specifically notes experiencing flare-ups on the back of her legs, her face, and in the creases of her elbows. This personal experience has led her to a place of acceptance: "I’ve had to learn not to hide it or feel embarrassed. It’s just part of who I am." This sentiment underscores a broader challenge for individuals with visible chronic conditions, particularly those in professions that demand public presentation.
Unraveling the Triggers of Eczema Flare-ups
One of the most confounding aspects of eczema is the wide-ranging nature of its triggers, which can not only differ between individuals but also change for the same person over time. McMahan has found her triggers have shifted with age, contributing to the unpredictable nature of her flare-ups. This unpredictability highlights the critical role of consulting with a knowledgeable dermatologist who can accurately diagnose eczema and develop a personalized management strategy.
"When I was younger, I noticed certain fabrics or detergents would set things off," McMahan recalled. "These days, it’s more stress and weather changes. I’ll think I have it all figured out, and then winter hits—or I’m traveling a lot—and my eczema will flare up." This sentiment, "Eczema can really keep you guessing," encapsulates the frustration many experience. Beyond personal factors like stress and weather, other common triggers identified by the National Institute of Allergy and Infectious Diseases include fragrances, cigarette smoke, certain skincare products, and environmental irritants such as mold and pollen. The constant vigilance required to identify and avoid these triggers can be emotionally and physically taxing.
Understanding Eczema Presentation Across Diverse Skin Tones
The visual presentation of eczema is not uniform, and skin tone can significantly influence how flare-ups appear. Symptoms can range from red or inflamed rashes and scaly patches to fluid-filled blisters or thickened, leathery skin over time. This variability in appearance emphasizes the necessity for close collaboration between patients and dermatologists for accurate diagnosis and effective management.
McMahan has adopted a proactive approach, diligently tracking her triggers, simplifying her skincare and makeup routines, and maintaining open lines of communication with her dermatologist. "Communication with your healthcare provider can be key," she stated. "I’ve learned to speak up when something’s not working, rather than just powering through a flare." This patient-advocacy approach is crucial, particularly as research continues to highlight disparities in how dermatological conditions are diagnosed and treated across different skin tones. Ensuring that healthcare providers are educated on the varied presentations of eczema on all skin types is an ongoing area of focus within the medical community.
Exploring Treatment Avenues with Dermatological Expertise
Given the wide spectrum of eczema symptoms and flare-up patterns, a one-size-fits-all treatment approach is rarely effective. Dermatologists play a pivotal role in diagnosing the specific type of eczema a patient has and crafting an individualized treatment plan tailored to their unique needs and symptom profile.
For McMahan, this personalized plan includes OPZELURA® (ruxolitinib) cream, a non-steroidal, prescription cream applied twice daily. OPZELURA is FDA-approved for the short-term and non-continuous chronic treatment of mild to moderate eczema in individuals aged 2 years and older whose condition is not adequately controlled by topical prescription therapies, or when such therapies are not recommended. It is important to note that the use of OPZELURA in conjunction with therapeutic biologics, other JAK inhibitors, or potent immunosuppressants is not advised. Safety and efficacy in children under 2 years of age with atopic dermatitis have not been established.

McMahan expressed particular interest in OPZELURA due to its steroid-free nature and its suitability for use on sensitive areas, as advised by her dermatologist. "I’ve tried different eczema treatments over the years, including topical steroids, and nothing felt like the right option for me," she admitted. "When my dermatologist mentioned OPZELURA, I decided to give it a try." The relief she experienced upon seeing her skin begin to clear was palpable: "It’s great to know that if I have a flare-up, I can use OPZELURA to help manage my symptoms. I have something to grab the minute I feel a flare-up coming on." This sentiment reflects a common desire among eczema patients for effective, non-intrusive treatment options that can be readily deployed at the first sign of a flare.
The Importance of Patient Education and Support
The journey with eczema is often a long and challenging one, requiring ongoing management and adaptation. Resources like MyMomentsOfClarity.com aim to provide a platform for individuals living with mild to moderate eczema to share their experiences and find inspiration for relief. These platforms are vital for fostering a sense of community and shared understanding, offering practical advice and emotional support that can complement medical treatment.
The medical community continues to advance its understanding of AD, with ongoing research focusing on the underlying immune pathways and the development of novel therapeutic targets. This includes exploring the role of the skin barrier, the microbiome, and the complex signaling networks that contribute to inflammation and itching. Furthermore, there is a growing emphasis on a holistic approach to eczema management, incorporating not only pharmacological interventions but also lifestyle modifications, stress management techniques, and patient education.
Critical Safety Information and Considerations for OPZELURA
While OPZELURA offers a promising treatment option for many, it is crucial for patients and healthcare providers to be aware of its safety profile. OPZELURA is a prescription medicine intended for topical use only. It is not intended for use in the eyes, mouth, or vagina.
Potential Serious Side Effects of OPZELURA:
- Serious Infections: OPZELURA contains ruxolitinib, a JAK inhibitor. These medications can suppress the immune system, increasing the risk of serious infections, including tuberculosis (TB), and fungal, bacterial, or viral infections that can spread throughout the body. Hospitalizations and fatalities have occurred due to these infections. Patients may be at increased risk of shingles (herpes zoster). Close monitoring for signs and symptoms of infection, including TB, is essential. OPZELURA should not be initiated in individuals with active, serious infections.
- Increased Risk of Death: In individuals aged 50 years and older with at least one cardiovascular risk factor taking oral JAK inhibitors, an increased risk of death from any cause has been observed.
- Cancer and Immune System Problems: OPZELURA may increase the risk of certain cancers, including lymphoma and lung cancer, particularly in current or past smokers. Non-melanoma skin cancers have also been reported. Regular skin checks by a healthcare provider are recommended, and limiting sun exposure while using protective clothing and sunscreen is advised.
- Increased Risk of Major Cardiovascular Events: Oral JAK inhibitors have been associated with an increased risk of major cardiovascular events, such as heart attack and stroke, in individuals aged 50 and older with at least one cardiovascular risk factor, especially in smokers.
- Blood Clots: The risk of blood clots in the veins of the legs (deep vein thrombosis, DVT) or lungs (pulmonary embolism, PE) can be increased with OPZELURA. These can be life-threatening. The risk is higher in individuals aged 50 and older with at least one cardiovascular risk factor taking oral JAK inhibitors.
- Low Blood Cell Counts: OPZELURA can potentially cause reductions in platelet counts (thrombocytopenia), red blood cell counts (anemia), and white blood cell counts (neutropenia, lymphopenia, leukopenia). Blood tests to monitor cell counts may be necessary, and treatment may be discontinued if significant reductions occur.
- Cholesterol Increases: While more commonly associated with oral ruxolitinib, increases in cholesterol levels have been observed. Patients with pre-existing high cholesterol or triglycerides should inform their healthcare provider.
Before starting OPZELURA, patients should inform their healthcare provider about all medical conditions, including any infections, history of cancer, heart problems, blood clots, or immune system issues. A comprehensive discussion of all medications, including prescription drugs, over-the-counter medicines, vitamins, and herbal supplements, is also critical to avoid potential interactions.
Common side effects of OPZELURA for atopic dermatitis include: nasopharyngitis, diarrhea, bronchitis, ear infection, increased eosinophil count or decreased neutrophil count, hives, folliculitis, tonsillitis, rhinorrhea, upper respiratory tract infection, COVID-19, fever, and application site reactions such as pain, irritation, discomfort, or itching.
Patients are encouraged to report any adverse reactions to their healthcare provider and to the FDA at 1-800-FDA-1088 or Incyte Corporation at 1-855-463-3463. The Full Prescribing Information, including the Boxed Warning and Medication Guide for OPZELURA, should be reviewed thoroughly.
This article was created in partnership with Incyte. All patient experiences and quotes reflect personal opinions. Heather McMahan was compensated for her participation.