USC Study Reveals Link Between Elevated Brain Iron Levels and Accelerated Alzheimer’s Progression in Down Syndrome Patients
Researchers at the USC Leonard Davis School of Gerontology have identified a critical biological mechanism that explains why individuals with Down syndrome are disproportionately affected by early-onset Alzheimer’s disease. The study, published by a team of neurobiologists and gerontologists, establishes a direct correlation between abnormally high concentrations of iron in the brain and increased oxidative damage to cell membranes. This specific form of cellular degradation, known as ferroptosis, appears to be a primary driver of the accelerated cognitive decline observed in patients who carry both a Down syndrome diagnosis and Alzheimer’s pathology.
The findings represent a significant shift in the understanding of neurodegenerative progression. While the presence of amyloid-beta plaques has long been the hallmark of Alzheimer’s research, this study suggests that iron-mediated toxicity may be the "missing link" that explains the unique severity and early arrival of symptoms in the Down syndrome population. By analyzing donated brain tissue, the researchers found that individuals with Down syndrome and Alzheimer’s disease (DSAD) possessed iron levels twice as high as those found in the brains of individuals with Alzheimer’s alone or those with no neurodegenerative conditions.
The Biological Intersection of Down Syndrome and Alzheimer’s
Down syndrome, or Trisomy 21, is a genetic condition characterized by the presence of a third copy of chromosome 21. This chromosomal anomaly is the root cause of the early-onset Alzheimer’s seen in this demographic because chromosome 21 houses the gene for the amyloid precursor protein (APP). In the general population, two copies of this gene regulate the production of proteins essential for neuronal growth and repair. However, the extra copy in individuals with Down syndrome leads to a chronic overproduction of APP.
When APP is processed by enzymes, it creates amyloid-beta (Aβ), a "sticky" protein fragment that aggregates into plaques. These plaques disrupt communication between neurons and eventually lead to cell death. Because of this genetic "overdose," approximately 50% of individuals with Down syndrome show clinical signs of Alzheimer’s disease by the age of 60—a full two decades earlier than the average age of onset in the general population.
"This makes understanding the biology of Down syndrome incredibly important for Alzheimer’s research," said University Professor Emeritus Caleb Finch, the study’s senior author. The research team posits that the extra APP gene does not just increase plaque formation but also fundamentally alters how the brain manages metallic elements like iron, creating a toxic environment that hastens the destruction of the prefrontal cortex.
Ferroptosis: A New Frontier in Neurodegeneration
The USC study specifically highlights the role of ferroptosis, a relatively recently discovered form of programmed cell death that is distinct from apoptosis. Ferroptosis is characterized by the iron-dependent accumulation of lipid peroxides—essentially, the "rusting" of the fatty membranes that protect brain cells.
Max Thorwald, the study’s lead author and a postdoctoral fellow in Finch’s laboratory, explained that the buildup of iron drives a cascade of oxidative stress. "Essentially, iron builds up, drives the oxidation that damages cell membranes, and overwhelms the cell’s ability to protect itself," Thorwald stated.
The research team focused their investigation on the prefrontal cortex, the brain’s executive center responsible for complex cognitive behavior, decision-making, and social regulation. By comparing brain tissues across three groups—healthy controls, Alzheimer’s patients, and DSAD patients—they discovered that the DSAD group exhibited a "perfect storm" of cellular failure. Not only was the iron concentration doubled, but the levels of protective antioxidant enzymes were significantly depleted, leaving the neurons defenseless against the corrosive effects of the iron.
Lipid Rafts as Hotspots for Brain Damage
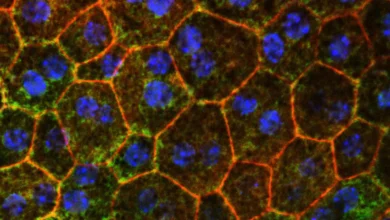
A key component of the study involved the examination of "lipid rafts." These are specialized microdomains within the cell membrane that serve as organizational hubs for signaling proteins. They are particularly crucial in the brain because they regulate how APP is cleaved into the toxic amyloid-beta proteins.
The USC researchers found that in the brains of those with DSAD, these lipid rafts were heavily compromised. They showed significantly higher levels of oxidative damage and a marked increase in the activity of β-secretase, the enzyme responsible for the first step in producing amyloid-beta.
The implications of this finding are profound: the damage caused by iron to the lipid rafts creates a feedback loop. As the rafts become more damaged by oxidation, they become more efficient at producing the very proteins that cause Alzheimer’s plaques. This suggests that the early cognitive decline in Down syndrome is not just a result of having more APP, but a result of the brain’s structural components being chemically altered to produce toxic proteins at an accelerated rate.
Comparative Data: The Role of Mosaic Down Syndrome
One of the most compelling pieces of evidence supporting the iron-APP connection came from the study of "mosaic" or "partial" Down syndrome. In these rare cases, only a percentage of the body’s cells contain the extra copy of chromosome 21, while others remain typically diploid.
The researchers observed that individuals with mosaic Down syndrome had significantly lower levels of both APP and iron in their brain tissue compared to those with full Trisomy 21. Consequently, these individuals tended to live longer and showed a delayed onset of Alzheimer’s symptoms. This "dose-response" relationship provides strong evidence that the quantity of APP—and the subsequent iron accumulation it triggers—is the primary variable in determining the speed of neurodegeneration.
"These cases really support the idea that the amount of APP—and the iron that comes with it—matters a lot in how the disease progresses," Finch noted. This finding narrows the focus for future researchers, pointing directly at iron regulation as a viable target for medical intervention.
A Chronology of Understanding the DS-AD Link
The relationship between Down syndrome and Alzheimer’s has been a subject of scientific inquiry for nearly a century, though the USC study provides the most detailed look at the chemical mechanics to date.
- 1866: John Langdon Down first describes the clinical features of the syndrome that would later bear his name.
- 1906: Alois Alzheimer identifies the plaques and tangles that characterize the disease.
- 1960s-70s: Pathologists begin to notice that nearly all adults with Down syndrome over the age of 40 have the same brain plaques as elderly Alzheimer’s patients.
- 1984: Researchers identify the APP gene on chromosome 21, establishing the genetic link between the two conditions.
- 2012: The term "ferroptosis" is coined, providing a name for the iron-dependent cell death observed in various diseases.
- 2024: The USC Leonard Davis School of Gerontology team publishes findings confirming that iron levels in DSAD brains are twice as high as in standard Alzheimer’s cases, identifying ferroptosis as a primary driver of the disease.
Clinical Implications and the Future of Treatment
The discovery of iron’s role in DSAD opens the door to new therapeutic strategies that move beyond the current focus on amyloid-clearing drugs. While several recently approved Alzheimer’s treatments focus on removing existing plaques, they have shown limited efficacy in reversing cognitive decline, particularly in advanced stages.
The USC team suggests that iron-chelating treatments could be a game-changer. Iron chelation involves the administration of compounds that bind to excess metal ions, allowing them to be safely excreted from the body. Preliminary studies in animal models have shown that reducing brain iron can lower the markers of Alzheimer’s pathology and improve cognitive function.
"Medications that remove iron from the brain or help strengthen antioxidant systems might offer new hope," Thorwald said. This approach would be prophylactic—aimed at preventing the "rusting" of the brain before the damage becomes irreversible. For the Down syndrome community, which faces an almost certain risk of Alzheimer’s, early intervention with iron-regulating therapies could potentially delay the onset of dementia by years or even decades.
Analysis: A Broader Impact on Aging Research
The implications of this study extend far beyond the Down syndrome community. Because people with Down syndrome develop Alzheimer’s in a more "distilled" and predictable genetic fashion, they provide researchers with a clearer window into the disease’s progression. What is learned from studying DSAD often applies to the general population.
If iron-mediated ferroptosis is a major driver of Alzheimer’s in Down syndrome, it is highly likely a contributing factor in "sporadic" Alzheimer’s (the form that affects the general elderly population). This research reinforces a growing consensus in gerontology that neurodegeneration is a multi-factorial process involving genetics, metallic toxicity, and the failure of cellular repair mechanisms.
Furthermore, the study highlights the importance of personalized medicine. By understanding that certain populations have specific biological vulnerabilities—such as the iron-sensitivity seen in Trisomy 21—doctors can tailor preventative care.
Support and Funding
The study was a collaborative effort involving multiple institutions and was supported by extensive federal and private funding. Major contributors included the National Institute on Aging (NIA) and various branches of the National Institutes of Health (NIH). Additional support was provided by the Cure Alzheimer’s Fund, the Simons Collaboration on Plasticity in the Aging Brain, the Larry L. Hillblom Foundation, the Glenn Foundation for Medical Research, and the Navigage Foundation.
This broad base of support underscores the scientific community’s recognition that solving the mystery of Alzheimer’s in the Down syndrome population is a critical step toward solving the Alzheimer’s crisis at large. As researchers move toward clinical trials involving iron regulation, the findings from the USC Leonard Davis School of Gerontology will serve as a foundational roadmap for the next generation of neuroprotective therapies.