Are vegetable and seed oils “toxic”?!
The modern dietary landscape is a battleground of conflicting advice, and few topics ignite as much fervent debate as the humble cooking oil. From viral social media posts on platforms like TikTok to the shelves of best-selling health books, the assertion that vegetable oils—often collectively dubbed "seed oils"—are inherently "toxic" has gained considerable traction. This narrative, amplified by proponents of diets such as the carnivore diet, frequently paints these common kitchen staples as "toxic sludge," "motor oil," or "the hateful eight," alleging they are the primary, yet unrecognized, drivers of chronic disease.
Historical Roots of a Contentious Debate
The discussion surrounding vegetable oils is far from new. Their introduction into the marketplace over a century ago immediately sparked questions about their nutritional value and safety. Historically, animal fats like butter and lard were primary cooking mediums. The early 20th century saw the emergence of vegetable oils and products like margarine, often marketed as healthier, more affordable alternatives to animal fats. This shift was partly fueled by industrial innovation and partly by evolving—and sometimes misguided—dietary science that demonized saturated fats while promoting alternatives. The initial promise was that these new fats would safeguard heart health, a claim that would later become a focal point of intense scrutiny.
The modern resurgence of the "toxic seed oil" theory, however, often frames their widespread adoption as a profit-driven scheme by corporations to sell cheap-to-grow crops to an unsuspecting public. Critics argue that, much like the controversial rise of trans-fat-laden margarine, vegetable oils were erroneously promoted as superior to traditional fats like butter, only to reveal themselves as worse culprits, linked to a litany of modern ailments including obesity, anxiety, depression, and inflammatory conditions like ulcerative colitis.
Conversely, a substantial body of scientific and nutritional experts maintains that many vegetable oils are either harmless or, in fact, health-promoting, particularly when consumed as part of a balanced diet and used in appropriate culinary contexts. They often highlight their benefits over saturated animal fats. This stark dichotomy leaves consumers adrift, wondering which perspective holds the truth. As is often the case in nutrition, the reality is far more intricate than any soundbite or meme can convey, demanding a nuanced, evidence-based examination.
Demystifying "Vegetable Oils": A Clarification of Terms
To navigate this complex debate, it’s crucial to first understand what constitutes a "vegetable oil" in the context of this discussion. Often used interchangeably with "seed oils," these fats are, as their name suggests, derived from the seeds of various plants. The most common examples found on typical grocery store shelves include:
- Canola oil (from rapeseed)
- Soybean oil
- Corn oil
- Sunflower oil
- Safflower oil
- Cottonseed oil
- Grapeseed oil
- Rice bran oil
It’s important to note that many other commonly used cooking oils, such as olive oil, avocado oil, palm oil, and coconut oil, are typically not categorized as "vegetable" or "seed" oils in this specific debate. These oils are extracted from the fruit flesh rather than the seed, and their distinct fatty acid profiles and processing methods often place them in a different nutritional conversation.
The Industrial Journey: How Vegetable Oils Are Processed
The distinction between seed oils and fruit-derived oils like olive or avocado oil extends significantly to their extraction methods. Olives and avocados are naturally rich in fat, allowing for relatively simple mechanical extraction, such as cold pressing, to yield oil. In theory, one could even produce olive oil at home with basic equipment.
The same cannot be said for most seed oils. Seeds like corn or soybeans possess a comparatively low fat content, necessitating a far more intensive, multi-step industrial process to efficiently extract the oil. This journey typically involves several key stages:
- Cleaning and Grinding: Seeds are cleaned and then ground into a meal to increase the surface area for oil extraction.
- Pre-pressing (Optional): Some seeds, like canola, may undergo an initial mechanical pressing (expeller pressing) to remove a portion of the oil. This is often done without high heat or chemical solvents for "expeller-pressed" varieties.
- Solvent Extraction: For most conventional seed oils, the remaining oil is extracted using chemical solvents, most commonly hexane. This maximizes oil yield from the low-fat seed meal.
- Desolventizing: The hexane is then evaporated from the crude oil, and the seed meal is also processed to remove residual solvent.
- Degumming: Water is added to remove phospholipids (gums), which can cause cloudiness and unwanted flavor.
- Refining (Neutralization): The oil is treated with an alkali solution to remove free fatty acids, which contribute to off-flavors and odors. This step significantly improves the oil’s stability and shelf life.
- Bleaching: The oil is treated with activated clays or carbons to remove pigments, resulting in a lighter, clearer appearance.
- Deodorizing: The final, most aggressive step involves steam distillation under high vacuum and temperature to remove volatile compounds that cause undesirable odors and flavors. This process can be quite harsh.
This extensive processing has significant implications for the oil’s nutritional profile. Crucially, health-promoting compounds such as polyphenols, tocopherols (Vitamin E), and other antioxidants are largely stripped away during refining. Furthermore, the high heat and chemical treatments can alter the delicate unsaturated fatty acids, leading to the formation of trans fatty acids (also known as partially hydrogenated fat) and oxidized lipid byproducts. While the Food and Drug Administration (FDA) banned manufacturers from adding trans fats to processed foods in 2018 due to their well-established links to heart disease, small amounts can still be formed incidentally during the high-temperature processing of refined vegetable oils or during prolonged deep frying, where oils are subjected to repeated heating cycles. To label these processed oils as "toxic" might be an overstatement, but the scientific consensus unequivocally advises minimizing trans fat intake, making the incidental formation a valid concern.

The "Toxic" Claims: Deconstructing the Anti-Seed Oil Argument
The primary criticisms leveled against seed oils revolve around their high content of polyunsaturated omega-6 fatty acids, particularly linoleic acid, and their susceptibility to oxidation during processing and cooking.
The argument posits that human diets historically featured a much lower ratio of omega-6 to omega-3 fatty acids, perhaps closer to 1:1 or 4:1. Modern Western diets, rich in refined seed oils and ultra-processed foods, often exhibit ratios as high as 16:1 or 20:1. Critics suggest this imbalance promotes a pro-inflammatory state in the body, potentially increasing the risk of chronic inflammatory diseases, cardiovascular disease, and metabolic disorders. The theory is that omega-6 fatty acids, when in excess and unbalanced with omega-3s, can be metabolized into pro-inflammatory eicosanoids.
Furthermore, polyunsaturated fats, by their chemical structure, are more prone to oxidation when exposed to heat, light, and air compared to monounsaturated or saturated fats. As mentioned, the refining process strips away natural antioxidants that would otherwise protect these delicate fatty acids. When oxidized, these lipids can form harmful compounds that are hypothesized to contribute to cellular damage and inflammation, thereby increasing the risk of various health conditions.
The Counter-Narrative: Nuance and Evidence-Based Perspectives
While the concerns about processing and omega-6 ratios are valid points for discussion, the scientific community’s view on seed oils is more nuanced. Many experts highlight that not all vegetable oils are created equal, and the context of their consumption is paramount.
For instance, certain vegetable oils, particularly those labeled "high-oleic," have been specifically bred to contain a higher proportion of monounsaturated fatty acids (MUFAs), similar to olive oil, making them more stable and less prone to oxidation. Expeller-pressed varieties also retain more beneficial compounds due to less harsh processing.
Regarding the omega-6 debate, the scientific consensus has evolved. While a massive imbalance is undesirable, recent comprehensive reviews, including a 2019 study published in the American Heart Association journal Circulation, have found that replacing saturated fats with omega-6 rich polyunsaturated fats actually reduced the risk of cardiovascular events, stroke, and early death. Harvard Health, echoing this sentiment, has published articles titled "No need to avoid healthy omega-6 fats."
The key distinction, many scientists argue, lies in the source of omega-6s. When consumed as part of whole foods like nuts and seeds, which come packaged with fiber, protein, vitamins, minerals, and a complex matrix of antioxidants, omega-6 fatty acids are associated with numerous health benefits, including reduced inflammation and improved cholesterol levels. The problem arises when omega-6s are consumed in isolation as highly refined oils, devoid of their protective co-factors, and often within a diet dominated by ultra-processed foods.
Expert Recommendations: A Balanced Approach to Dietary Fats
Precision Nutrition, a leading authority in health and fitness coaching, offers a structured approach to dietary fats, categorizing them to guide informed choices. Their visual guides, designed to help individuals make sensible decisions, place fats into three tiers: "Eat More," "Eat Some," and "Eat Less."
"Eat More" Category: This category emphasizes fats with robust scientific backing for their health-promoting properties.
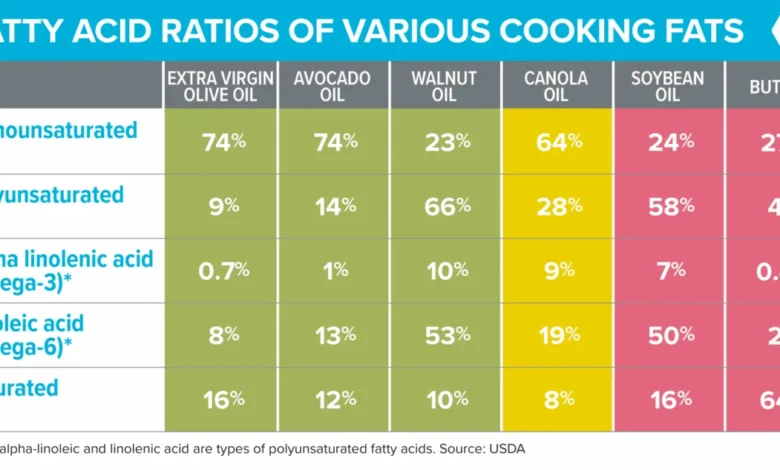
- Extra Virgin Olive Oil (EVOO): This is a standout recommendation. EVOO is mechanically pressed from olives without heat or chemical solvents, preserving its rich content of heart-healthy monounsaturated fatty acids (MUFAs) and potent polyphenols. These plant-based compounds are powerful antioxidants and anti-inflammatory agents. Extensive research, particularly studies on the Mediterranean diet, consistently links higher EVOO consumption to a reduced risk of cardiovascular disease, stroke, certain cancers (e.g., breast cancer), type 2 diabetes, and even neurodegenerative diseases like Alzheimer’s. Its stability, even at cooking temperatures (up to 410°F or 210°C), due to its antioxidant profile, dispels older myths about its unsuitability for cooking.
- Avocado Oil (Cold-pressed): Similar to EVOO, cold-pressed avocado oil is rich in MUFAs and antioxidants, making it another excellent choice for cooking and dressings.
- Walnut Oil: Valued for its omega-3 content, it’s best used in dressings due to its lower heat stability.
"Eat Some" Category: This category includes oils that are generally considered health-neutral or mildly beneficial when consumed in reasonable amounts.

- Expeller-Pressed Canola Oil: Made from rapeseed through mechanical pressing, this method avoids harsh chemical solvents and high heat, preserving more of its beneficial compounds, including monounsaturated fats and alpha-linolenic acid (ALA), a plant-based omega-3 fatty acid. While not as extensively studied as EVOO, expeller-pressed canola oil can be a budget-friendly, neutral-flavored option suitable for baking and moderate-heat cooking. Its phytosterols are also known to help influence blood cholesterol positively when used as a substitute for saturated fats.
- High-Oleic Sunflower and Safflower Oils: These are specific varieties bred to be high in monounsaturated fats, making them more stable and healthier than their conventional, high-linoleic counterparts.
"Eat Less" Category: This category includes fats that should be limited due to potential health concerns, especially when consumed in large quantities or as part of a highly processed diet.
- Refined Vegetable Oils: This includes conventional corn, soybean, sunflower, and safflower oils (not high-oleic). Their extensive refining process strips beneficial compounds and can lead to the formation of trans fats and oxidized lipids.
- Butter and other Saturated Fats: While not inherently "toxic," excessive intake of saturated fat (beyond 10% of total daily calories) is associated with elevated LDL cholesterol and increased risk of heart disease. Butter, in particular, has a lower concentration of the protective milk fat globule membrane found in other dairy products, meaning it can raise blood cholesterol more significantly than full-fat milk or yogurt.
Head-to-Head: Key Oil Comparisons and Their Implications
Extra Virgin Olive Oil vs. Expeller-Pressed Canola Oil:
EVOO emerges as the clear winner due to its superior fatty acid profile, rich antioxidant content, and an overwhelming body of research supporting its cardiovascular and anti-inflammatory benefits. For example, a large study of over 22,000 adults in Southern Italy found that those consuming more than two tablespoons of olive oil daily had a 20% lower mortality risk over 13 years compared to those consuming less than one tablespoon. However, expeller-pressed canola oil offers a more affordable, flavor-neutral alternative for baking or budget-conscious consumers, and when used in moderation, it is considered at least health-neutral, if not slightly beneficial.
Expeller-Pressed Canola Oil vs. Refined Canola Oil:
Expeller-pressed canola oil wins this matchup by a small margin. The mechanical pressing process avoids harsh chemicals and high heat, thus preserving more of its beneficial alpha-linolenic acid (omega-3) and phytosterols. Refined canola oil, conversely, loses some of these protective compounds and can contain small amounts of incidentally formed trans fatty acids, making it a less optimal choice. This highlights the importance of discerning processing methods when selecting oils.
The Omega-6 Dilemma Revisited:
The notion that omega-6 fatty acids are inherently inflammatory requires careful consideration. While an excessively high omega-6 to omega-3 ratio is not ideal, the primary concern lies with omega-6s from highly processed sources rather than whole foods. Nuts and seeds, naturally rich in omega-6s, are consistently linked to reduced blood cholesterol and inflammation, underscoring the "food matrix effect." These whole foods provide a synergistic blend of nutrients that mitigate potential downsides of isolated omega-6s. Refined vegetable oils, however, lack these protective co-factors, making their high omega-6 content more contentious when consumed excessively.
Refined Vegetable Oil vs. Butter: A Stalemate in the "Eat Less" Category
This matchup frequently fuels the most heated online debates. Proponents of butter often argue against the historical vilification of saturated fats, citing the disastrous consequences of replacing butter with trans-fat-laden margarine in past decades. While some research suggests the link between saturated fat and heart disease is not as straightforward as once believed, the consensus from major health organizations, including the U.S. Dietary Guidelines, advises limiting saturated fat to less than 10% of total calories. A single tablespoon of butter contains approximately 7 grams of saturated fat, roughly one-third of the daily limit for a 2000-calorie diet. Moreover, butter contains minimal amounts of the protective milk fat globule membrane (MFGM) found in other dairy products, which seems to buffer the cholesterol-raising effects of saturated fat.
On the other side, refined vegetable oils, due to their polyunsaturated nature, are more susceptible to oxidation, especially during the harsh refining process and repeated heating (e.g., in commercial deep fryers or ultra-processed food manufacturing). This oxidation can lead to the formation of harmful compounds and contribute to systemic inflammation. Crucially, the biggest source of refined vegetable oils for most people is not home cooking but rather ultra-processed foods (UPFs). These foods, ranging from packaged snacks to frozen meals, are not only loaded with refined oils but also typically high in added sugars, sodium, and artificial ingredients, while being devoid of beneficial fiber, vitamins, and minerals. Studies have linked high consumption of UPFs to an increased risk of premature death, heart disease, stroke, obesity, type 2 diabetes, cancer, and depression. The combination of oxidized oils within a nutrient-poor, hyper-palatable matrix makes UPFs a significant public health concern.
Ultimately, this specific comparison often results in a draw, with both refined vegetable oils and butter best consumed in moderation. Refined vegetable oils are often unbalanced in fatty acid profiles and stripped of protective compounds, with the potential for trans fat formation and oxidation. Butter, while less processed, is high in saturated fat and lacks the protective MFGM. The broader implication is that neither should form the cornerstone of a healthy diet, and both are best limited.
Broader Implications and Actionable Dietary Strategies
The discussion around cooking oils underscores a fundamental principle of nutrition: the overall dietary pattern is far more important than any single ingredient. Focusing on the following strategies can yield significant health benefits:
- Prioritize Minimally-Processed Whole Foods: Foods like nuts, seeds, avocados, olives, and fatty fish (e.g., salmon) provide healthy fats along with fiber, protein, vitamins, minerals, and a complex array of phytochemicals. These foods offer a "matrix effect" where nutrients work synergistically.
- Limit Ultra-Processed Foods (UPFs): Given that UPFs are the primary source of refined vegetable oils for many, reducing their consumption is a powerful step. UPFs are typically characterized by long ingredient lists including unfamiliar chemicals, lack of resemblance to their original food source, and industrial manufacturing. Aim for a diet where at least 80% of calories come from whole or minimally processed foods.
- Minimize Deep-Fried Foods: Regardless of the oil used, deep-frying subjects fats to extreme temperatures for prolonged periods, leading to oxidation and the formation of potentially harmful compounds. Fried foods should be relegated to the "eat less" category.
- Derive Most Fats from Food, Not Isolated Oils: While certain oils like EVOO can be health-promoting, the bulk of dietary fat should ideally come from whole food sources. These provide satiety, fiber, and a full spectrum of micronutrients that oils lack. A reasonable intake of 1-3 servings of oils or butter per day can fit into a healthy diet, but balance is key.
In conclusion, the debate surrounding vegetable and seed oils is multifaceted, with valid points on both sides. While some refined seed oils, particularly when heavily processed and consumed in ultra-processed foods, warrant caution, the blanket condemnation of all vegetable oils is an oversimplification. Extra virgin olive oil and cold-pressed avocado oil stand out as scientifically supported health-promoting choices. For those seeking budget-friendly or flavor-neutral options, expeller-pressed canola oil and high-oleic sunflower/safflower oils can be acceptable in moderation. Ultimately, a balanced diet rich in whole, minimally processed foods remains the most robust strategy for optimal health, naturally modulating fat intake and reducing exposure to potentially harmful compounds.
References
Click here to view the information sources referenced in this article. (This is a placeholder as per instructions; actual links would be provided in a real publication).