Smart Bandage a-Heal Utilizes AI and Bioelectronics to Accelerate Wound Recovery by Twenty-Five Percent
In a significant leap forward for regenerative medicine and wearable technology, a multidisciplinary team of engineers and researchers from the University of California, Santa Cruz (UCSC) and the University of California, Davis (UC Davis) has unveiled a revolutionary "smart bandage" known as a-Heal. This sophisticated wearable device integrates high-resolution imaging, artificial intelligence, and bioelectronic delivery systems to monitor and treat wounds in real-time. By automating the diagnostic and therapeutic process, the system has demonstrated the ability to accelerate the healing of acute wounds by approximately 25% compared to conventional standards of care, offering a glimpse into the future of personalized, remote healthcare.
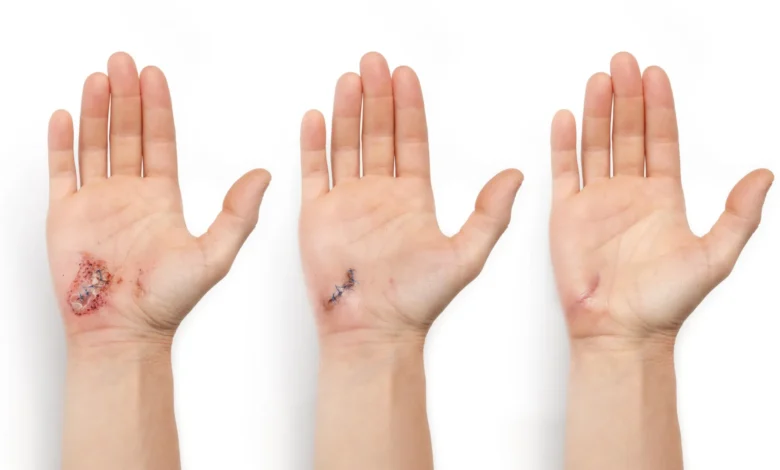
The development of a-Heal addresses a critical challenge in modern medicine: the variability of biological recovery. As a wound heals, it undergoes a complex, multi-stage progression involving clotting to stop bleeding, an immune system response to prevent infection, the formation of a scab, and finally, the remodeling of tissue known as scarring. Traditional bandages are passive, providing only a physical barrier against external contaminants. In contrast, the a-Heal system is an "active" or "closed-loop" device, meaning it can sense the state of the wound and respond with specific interventions without requiring constant human oversight.
The Architecture of a Closed-Loop Healing System
The a-Heal device represents one of the first successful integrations of a camera, machine learning, and bioelectronic actuators into a single, portable unit for wound management. The project was spearheaded by Marco Rolandi, the Baskin Engineering Endowed Chair and Professor of Electrical and Computer Engineering (ECE) at UC Santa Cruz, alongside a team of specialists in applied mathematics and bioengineering. The research was conducted under the auspices of the DARPA-BETR (Bioelectronics for Tissue Regeneration) program, an initiative aimed at developing technologies that can provide the same level of care for complex tissue injuries as a modern intensive care unit, but in a wearable format.
At the core of the device is a miniature camera developed by Mircea Teodorescu, an Associate Professor of Electrical and Computer Engineering at UCSC. This "microscope in a bandage" is programmed to capture high-definition images of the wound site every two hours. These images are not merely for documentation; they serve as the primary data source for the system’s "AI physician."
While a single image provides a snapshot of a wound’s current state, the power of a-Heal lies in its ability to track longitudinal trends. By analyzing a series of images over time, the AI can detect subtle changes in tissue color, texture, and moisture levels—indicators that might be invisible to the naked eye or even to a human clinician during a brief daily checkup. This continuous monitoring allows the system to identify exactly which stage of healing the patient is in and whether the recovery is proceeding according to an optimal timeline.
The AI Physician: Reinforcement Learning and Deep Mapper
The intelligence behind a-Heal is driven by a reinforcement learning (RL) model developed by Marcella Gomez, an Associate Professor of Applied Mathematics at UCSC. Reinforcement learning is a subset of machine learning where an algorithm learns to achieve a goal through trial and error, receiving "rewards" for actions that bring it closer to the desired outcome—in this case, total wound closure in the shortest possible timeframe.
To bridge the gap between raw visual data and clinical decision-making, Gomez and her team developed a specialized algorithm called "Deep Mapper." This tool processes the wound images to quantify the healing stage relative to a normal progression model. By mapping the current state of the wound along a predicted trajectory, the AI can forecast future progress.
"It’s not enough to just have the image," Gomez explained during the announcement of the preclinical results. "You need to process that and put it into context. Then, you can apply the feedback control."
If the AI physician detects that the wound is lagging behind its expected healing trajectory, it initiates a therapeutic intervention. This feedback loop is what defines the "closed-loop" nature of the device. The system learns the specific biological responses of the individual patient in real-time, adjusting the dosage of medication or the intensity of an electric field to suit the unique needs of that person’s physiology.
Therapeutic Interventions: Bioelectronics and Biochemistry
The a-Heal device employs two primary methods of treatment: biochemical delivery and electrotherapy. Both methods are administered through bioelectronic actuators designed by the Rolandi Group at UCSC.
The primary medication delivered by the device is fluoxetine, a selective serotonin reuptake inhibitor (SSRI). While fluoxetine is widely known as an antidepressant, its topical application in wound care serves a different purpose. Research conducted by the Isseroff group at UC Davis has shown that serotonin levels within a wound site play a crucial role in the healing process. By controlling these levels topically, fluoxetine can decrease inflammation and promote faster tissue closure. The a-Heal system determines the precise concentration of the drug needed and delivers it directly to the wound bed.
In addition to pharmacological treatment, the device can apply a controlled electric field to the wound. This technique, developed through the work of Min Zhao and Roslyn Rivkah Isseroff at UC Davis, leverages a biological phenomenon known as galvanotaxis—the tendency of certain cells, such as skin cells and immune cells, to migrate along an electrical gradient. By optimizing the magnitude of the applied electric field, the a-Heal device effectively "guides" cells toward the center of the wound, accelerating the physical closure of the injury.
Preclinical Success and Supporting Data
The effectiveness of a-Heal was validated through a series of preclinical trials conducted at UC Davis. The results, which were published in the journal npj Biomedical Innovations, were striking. Wounds treated with the a-Heal system followed a recovery trajectory that was 25% faster than those treated with standard medical care.
Beyond the speed of closure, the researchers noted that the system was particularly effective at "jump-starting" wounds that had stalled in the inflammatory phase. This is a common issue in chronic wounds, such as diabetic ulcers or pressure sores, where the body’s natural healing process becomes "stuck," leading to long-term infections and, in severe cases, the need for amputation.
The data gathered during these trials showed that the AI’s ability to adjust treatment in real-time was superior to a static treatment plan. Because the device transmits its data and images to a secure web interface, human physicians can monitor the progress remotely. This allows for a "human-in-the-loop" approach where a doctor can intervene or fine-tune the AI’s parameters if necessary, though the preclinical trials demonstrated that the AI was highly capable of managing the process autonomously.
Chronology of Development and Research Milestones
The path to a-Heal involved years of interdisciplinary collaboration and several key research milestones:
- Conceptualization (DARPA-BETR Program): The project began with the goal of creating a "smart" alternative to traditional bandages for military and civilian use, focusing on complex tissue regeneration.
- Bioelectronic Actuator Development: Professor Marco Rolandi’s team perfected the delivery mechanisms for topical drugs and electrical stimulation.
- Visual Diagnostic Integration: Professor Mircea Teodorescu developed the specialized onboard camera and imaging protocols, later described in Communications Biology.
- AI and Reinforcement Learning Refinement: Professor Marcella Gomez and her students developed the Deep Mapper algorithm and the reinforcement learning framework, publishing their findings in the journal Bioengineering.
- Preclinical Testing: The UC Davis team, led by Professors Isseroff and Zhao, conducted the vital tests on wound models to prove the system’s efficacy.
- Full System Integration: The successful combination of these components into the a-Heal wearable, leading to the current published results in npj Biomedical Innovations.
Broader Impact and Healthcare Implications
The implications of a-Heal extend far beyond the laboratory. Chronic wounds represent a massive burden on global healthcare systems. In the United States alone, chronic wounds affect approximately 6.7 million people, with treatment costs exceeding $25 billion annually. As the prevalence of diabetes and obesity—both of which contribute to poor wound healing—continues to rise, the demand for advanced wound care solutions is becoming more urgent.
By providing a portable, wireless, and automated treatment system, a-Heal could democratize high-end medical care. Patients in remote or rural areas, who may not have easy access to wound care specialists, could use the device to receive hospital-grade treatment at home. Similarly, for patients with limited mobility or those in elderly care facilities, the device reduces the need for frequent, painful dressing changes and clinical visits.
Furthermore, the technology holds significant promise for military medicine. On the battlefield, immediate and effective wound management is critical for preventing infection and ensuring the long-term recovery of service members. A device that can autonomously manage a wound during the "golden hour" after an injury could save lives and limbs.
Future Research and Clinical Potential
While the current results are based on preclinical models, the research team is already looking toward the next phase of development. Future iterations of a-Heal will focus on managing infected wounds and exploring the use of additional biosensors to detect pH levels, temperature, and oxygenation at the wound site. These additional data points would provide the AI physician with an even more nuanced understanding of the healing environment.
"Our system takes all the cues from the body, and with external interventions, it optimizes the healing progress," Rolandi stated. The goal is to move toward clinical trials in humans, where the device’s ability to handle the complexities of human biology and varied environments will be the ultimate test.
As wearable technology continues to evolve from simple fitness trackers to sophisticated medical intervention tools, a-Heal stands as a landmark achievement. It demonstrates that by combining the "eyes" of bioelectronics with the "brain" of artificial intelligence, medicine can move away from a one-size-fits-all approach toward a truly personalized, responsive model of care. The successful integration of these technologies suggests a future where the bandage on a patient’s arm is as smart as the physician treating them, working tirelessly every two hours to ensure the fastest possible path to recovery.