American Heart Association Provides Critical Insights Following President Trumps Chronic Venous Insufficiency Diagnosis

The White House recently confirmed that President Donald J. Trump has been diagnosed with Chronic Venous Insufficiency (CVI), a common but often overlooked vascular condition. White House Press Secretary Karoline Leavitt announced the diagnosis following a series of medical evaluations prompted by the President experiencing mild swelling in his lower leg. According to the official statement, the clinical assessment included comprehensive laboratory testing and imaging, which returned results within normal limits, specifically ruling out more severe complications such as deep vein thrombosis (DVT) or peripheral arterial disease. In response to the high-profile diagnosis, the American Heart Association (AHA), the world’s leading nonprofit organization dedicated to heart and brain health, has issued a detailed briefing to educate the public on the implications of CVI, its relationship to cardiovascular health, and the importance of early intervention.
Understanding Chronic Venous Insufficiency
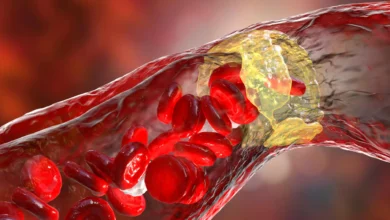
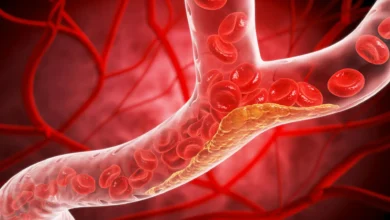
Chronic Venous Insufficiency is a manifestation of chronic venous disease that occurs when the venous wall or the valves in the leg veins do not function effectively. This dysfunction makes it difficult for blood to return to the heart from the limbs, causing blood to pool in the veins, a process known as stasis. Under normal physiological conditions, the muscles in the legs act as a pump to counteract gravity, while tiny valves inside the veins open and close to ensure blood flows in one direction: upward toward the heart. When these valves become weakened or damaged, blood can flow backward, leading to increased pressure within the venous system.
The American Heart Association emphasizes that CVI is highly prevalent, particularly among the aging population. Despite its frequency, the condition remains significantly underrecognized and undertreated in the United States. While often viewed as a cosmetic concern in its early stages—characterized by spider veins or mild varicose veins—the progression of CVI can lead to debilitating symptoms and is frequently an indicator of broader vascular instability.
The Cardiovascular Connection and Mortality Risk
One of the most critical aspects of the AHA’s recent communication is the established link between CVI and increased cardiovascular risk. Research indicates a strong association between the presence of chronic venous insufficiency and a higher risk of developing cardiovascular disease (CVD). Most notably, medical data suggests that CVI is a marker for increased mortality, independent of a patient’s age, sex, or existing comorbidities.
The presence of CVI often mirrors the presence of traditional cardiovascular risk factors, including advanced age, obesity, a sedentary lifestyle, and a history of smoking. For a public figure like President Trump, who is 78 years old, the diagnosis highlights the natural physiological challenges faced by the geriatric population. However, the AHA notes that because CVI is associated with clinically overt cardiovascular disease, its diagnosis should serve as a prompt for a comprehensive review of a patient’s overall heart health and vascular integrity.
Clinical Presentation and Symptoms
The diagnosis of President Trump followed reports of mild edema, or swelling, in the lower extremities. Edema is one of the hallmark symptoms of CVI and is typically most pronounced after long periods of standing or sitting. As the condition progresses, patients may experience a variety of symptomatic changes in the lower legs and ankles.
Commonly reported symptoms include:
- Varicose Veins: Enlarged, twisted veins that are visible just under the surface of the skin.
- Skin Alterations: Known as "venous eczema" or "stasis dermatitis," these appear as red, itchy, or scaly patches. Over time, the skin may become thick, leathery, or discolored (hyperpigmentation).
- Physical Discomfort: Patients often describe a feeling of heaviness, aching, or cramping in the legs. Throbbing, itching, and leg fatigue are also frequently cited.
- Restless Legs Syndrome: A common secondary symptom that can interfere with sleep and overall quality of life.
- Venous Ulcers: In advanced stages, poor circulation can lead to open sores, particularly around the ankles, which are difficult to heal and prone to infection.
Dr. Joshua A. Beckman, M.D., FAHA, a prominent vascular specialist and past volunteer chair of the American Heart Association’s Vascular Health Advisory Committee, stressed the importance of recognizing these signs early. "Chronic Venous Insufficiency can significantly impact your quality of life, but early detection and treatment can make a substantial difference," Dr. Beckman stated. He emphasized that awareness is the first step toward seeking the medical evaluation necessary to prevent the progression of the disease.
Diagnostic Procedures and the Exclusion of DVT
The White House’s transparency regarding the President’s diagnostic results—specifically the absence of deep vein thrombosis (DVT)—is a significant detail for medical professionals. DVT is a much more acute and dangerous condition where a blood clot forms in the deep veins of the leg. If a portion of such a clot breaks loose, it can travel to the lungs, causing a pulmonary embolism (PE), which can be fatal.
To differentiate between CVI and DVT, physicians utilize several advanced imaging techniques:
- Duplex Ultrasound: This is the primary tool for diagnosing CVI. It uses high-frequency sound waves to visualize the structure of the veins and measure the speed and direction of blood flow. It can pinpoint exactly where valves are leaking (reflux).
- Magnetic Resonance Venography (MRV): This imaging test uses a magnetic field and radio waves to provide detailed images of the veins, often used in complex cases to rule out obstructions or compressive syndromes in the pelvis.
- Computed Tomography Venography (CTV): This utilizes X-rays and contrast dye to create cross-sectional images, helping clinicians identify vein obstructions or structural abnormalities that may contribute to CVI.
In the case of President Trump, the use of these diagnostic tools allowed his medical team to confirm that while the valves in his veins may be experiencing insufficiency, there is no evidence of the life-threatening clots associated with DVT or the arterial blockages associated with peripheral artery disease.
Treatment and Management Strategies
The management of CVI focuses on improving blood flow and reducing the pressure within the veins. The American Heart Association outlines a multi-tiered approach to treatment, ranging from conservative lifestyle changes to minimally invasive surgical interventions.
Compression Therapy: This remains the cornerstone of CVI management. It involves the use of elastic garments, graded compression stockings, or multilayer bandages that apply consistent pressure to the legs. This pressure helps the vein valves function better and assists the "muscle pump" in moving blood back toward the heart. In some cases, pneumatic compression pumps—sleeves that inflate and deflate periodically—are used to stimulate circulation.
Pharmacological Interventions: While there is no "cure" for CVI in pill form, certain medications can manage symptoms. Topical anti-inflammatory steroids may be prescribed for skin irritation (stasis dermatitis), and diuretics may be used briefly to reduce significant swelling. In cases where venous ulcers have become infected, antibiotics are necessary.
Endovascular and Interventional Therapies: For patients who do not respond sufficiently to compression therapy, minimally invasive procedures are an option. These often involve endovenous laser ablation or radiofrequency ablation, where a catheter is inserted into the affected vein to seal it shut, redirecting blood flow to healthier veins. Other procedures include sclerotherapy, where a chemical solution is injected into the vein to cause it to collapse and eventually be absorbed by the body.
Broader Public Health Context
The diagnosis of a sitting or former President often brings national attention to specific health issues, and CVI is a condition that affects millions of Americans. According to the American Heart Association’s 2025 Heart Disease and Stroke Statistics, vascular diseases remain a leading cause of morbidity in the United States. The prevalence of CVI increases with every decade of life, and with an aging U.S. population, the economic and social burden of the disease is expected to rise.
The AHA’s proactive stance in sharing information following the White House announcement serves as a reminder that vascular health is an integral component of overall cardiovascular wellness. The organization advocates for regular physical activity—specifically exercises that strengthen the calf muscles—and weight management as primary preventative measures. For individuals with sedentary jobs or those who travel frequently (factors often associated with the presidency), the AHA recommends frequent movement breaks and the use of compression socks during long periods of inactivity.
Conclusion and Outlook
President Trump’s diagnosis of Chronic Venous Insufficiency, while requiring ongoing management, is a common condition among men and women of his age group. The White House’s report that his laboratory results were within normal limits and that no arterial disease or DVT was present suggests a manageable clinical path forward.
As Dr. Joshua A. Beckman noted, the goal of treatment is to maintain quality of life and prevent the more severe complications associated with the disease. By utilizing compression therapy and monitoring for skin changes, individuals with CVI can lead active, healthy lives. The American Heart Association continues to emphasize that while CVI is a distinct condition of the veins, its presence is a clear signal to remain vigilant about one’s broader heart health, ensuring that all cardiovascular risk factors are addressed through professional medical guidance.