Global Health Milestone: Over 60 Nations Now Integrate Refugees and Migrants into National Health Policies, WHO Report Reveals

The World Health Organization (WHO) has reported a significant paradigm shift in global responses to the health needs of refugees and migrants, with new data indicating that more than 60 countries – representing two-thirds of those surveyed – have now formally incorporated these vulnerable populations into their national health policies and laws. This landmark development, detailed in a comprehensive new report, establishes the first global baseline for systematically tracking progress toward the creation of inclusive, migrant-responsive health systems worldwide.
The Evolving Landscape of Human Migration and Health Challenges
Human migration has historically been, and continues to be, a fundamental driver of cultural, social, and economic evolution across generations. From ancient trade routes to modern globalized societies, the movement of people has shaped civilizations. Today, this phenomenon is more pronounced than ever, with over 1 billion individuals – exceeding one in eight people globally – living as refugees or migrants. This staggering figure encompasses a diverse array of circumstances and motivations, underscoring the complexity of modern human mobility.
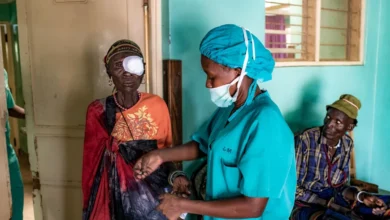
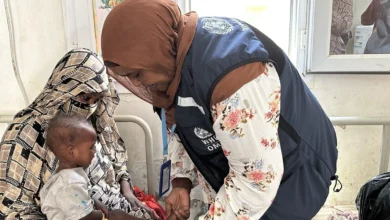
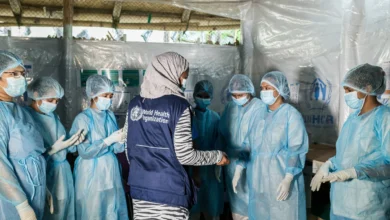
The reasons for such extensive movement are multifaceted and often intertwined. They range from acute crises such as armed conflict, political instability, and natural disasters (increasingly exacerbated by climate change) to the pursuit of economic opportunities, educational advancement, or family reunification. While many seek better lives or safety, the journey and subsequent settlement often expose refugees and migrants to a unique constellation of health risks and formidable barriers to accessing essential care. These challenges include, but are not limited to, heightened susceptibility to infectious diseases due to crowded living conditions or interrupted vaccination schedules, the exacerbation or development of chronic diseases due to stress and lack of continuity in treatment, significant mental health challenges stemming from trauma, loss, displacement, and the difficulties of integration, and exposure to unsafe living or working conditions in informal settlements or exploitative labor environments.
A Call for Universal Health Coverage: Dr. Tedros’s Vision
Dr. Tedros Adhanom Ghebreyesus, Director-General of the World Health Organization, articulated a powerful vision emphasizing the reciprocal relationship between refugees, migrants, and host communities. "Refugees and migrants are not just recipients of care, they are also health workers, caregivers and community leaders," Dr. Tedros stated, highlighting their active contributions to societies. He further underscored the foundational principle of universal health coverage, asserting, "Health systems are only truly universal when they serve everyone. WHO’s new report on the health of migrants and refugee shows that inclusion benefits whole societies and strengthens preparedness for future health challenges." This perspective positions the integration of migrant and refugee health as not merely a humanitarian imperative, but a strategic investment in the resilience and overall well-being of entire nations.
The WHO Report: A New Global Benchmark
The newly released "World report on promoting the health of refugees and migrants: monitoring progress on the WHO global action plan" represents a pivotal moment in global health governance. By drawing on extensive data collected from 93 Member States, the report provides an unprecedented, comprehensive overview of national policies and practices. Its significance lies in establishing the first verifiable global baseline, against which future progress in developing inclusive, migrant-responsive health systems can be consistently measured and tracked.
The report critically observes that even within politically sensitive and often contentious contexts surrounding migration, an increasing number of countries are demonstrating a reliance on robust evidence, disaggregated data, scientific principles, and established international norms and standards. This shift towards an evidence-based approach is guiding how migration and health considerations are integrated into national health systems, moving beyond ad-hoc responses to more structured and sustainable frameworks.
Far-Reaching Dividends of Investment in Inclusive Health Systems
Investing in the health of refugee and migrant populations yields substantial and far-reaching dividends that extend well beyond the immediate beneficiaries. Such investments actively support better social and economic integration, enabling individuals to contribute fully to their new societies through employment, taxation, and community engagement. Furthermore, they significantly strengthen the resilience of national health systems by preventing the spread of diseases, fostering a diverse healthcare workforce, and promoting overall public health. This aligns with the broader principle of global health security, recognizing that disease knows no borders and that "no one is safe until everyone is safe."
Inclusive, migrant-responsive health systems also demonstrate economic prudence by reducing long-term costs. By facilitating early access to preventive care and continuous treatment, these systems mitigate the need for more expensive emergency interventions later. Healthy and well-integrated populations are better positioned to participate economically and socially, transforming potential burdens into valuable contributors to the societies in which they reside. This proactive approach ensures a healthier populace and a more robust national economy.
Pioneering Initiatives: Case Studies from Across WHO Regions
The report illustrates practical progress through compelling case studies from all six WHO regions, showcasing how diverse nations are implementing inclusive policies:
-
Thailand’s Expanded Health Insurance Coverage: Thailand, a major destination for migrant workers primarily from neighboring Myanmar, Cambodia, and Laos, has made significant strides by expanding health insurance coverage for migrant populations. Historically, undocumented migrants faced immense barriers to healthcare, often delaying treatment until emergencies. Through a combination of national policies and voluntary schemes, Thailand has worked to integrate these populations into its public health system, recognizing the economic and public health benefits of a healthy migrant workforce. This has involved simplified registration processes and reduced costs, aimed at ensuring access to primary care, emergency services, and even some specialized treatments, thereby reducing financial barriers and promoting early intervention.
-
Belgium’s Cross-Cultural Communication Mediators: In Belgium, a country with a diverse immigrant population, the deployment of cross-cultural communication mediators has proven instrumental. These trained professionals bridge critical language and cultural gaps between healthcare providers and migrant patients. They facilitate accurate medical histories, ensure patient understanding of diagnoses and treatment plans, and help navigate cultural sensitivities around health beliefs and practices. This initiative is crucial in overcoming communication barriers that can otherwise lead to misdiagnosis, non-adherence to treatment, and a general distrust in the healthcare system, ultimately improving patient outcomes and satisfaction.
-
Chile’s Community-Led Primary Health Care: Chile has championed the inclusion of migrant community representatives in decision-making processes concerning primary health care delivery. By involving migrants directly in the planning and evaluation of health services, the country ensures that policies and programs are culturally appropriate, accessible, and genuinely responsive to the specific needs and priorities of these communities. This participatory approach fosters trust, empowers migrant populations, and leads to more effective and equitable health service provision, moving beyond a top-down model to one that is truly collaborative.
These examples underscore that despite varying national contexts and resource levels, progress towards more inclusive health systems is achievable through innovative and context-specific strategies.
Persistent Gaps and Remaining Challenges
Despite the encouraging progress highlighted in the report, significant gaps and persistent challenges continue to impede the full realization of health equity for refugees and migrants. These include:
- Inadequate Funding and Resource Allocation: Many countries still rely heavily on short-term humanitarian funding rather than integrating migrant and refugee health into sustainable national budgets. This leads to precarious service provision and a lack of long-term planning.
- Data Deficiencies: A pervasive lack of disaggregated data on the health status, access to services, and specific needs of refugee and migrant populations hinders evidence-based policymaking. Without robust data, it is challenging to identify vulnerable groups, allocate resources effectively, and measure the impact of interventions.
- Access Barriers Beyond Policy: Even where policies exist, practical barriers persist. These include administrative hurdles, language and cultural communication gaps, discriminatory practices by some healthcare providers, geographical remoteness of services, fear of deportation among undocumented migrants, and a general lack of awareness about available health services.
- Health Workforce Capacity: There is often a critical shortage of culturally competent healthcare professionals trained in migrant health issues. Many healthcare systems are not equipped to handle the diverse linguistic, cultural, and health literacy needs of migrant populations, leading to suboptimal care.
- Implementation Gaps: The existence of progressive policies on paper does not always translate into effective, equitable, and accessible services on the ground. Bureaucratic inertia, lack of political will, and insufficient training for frontline workers can derail well-intentioned policies.
- Mental Health Neglect: Mental health services for refugees and migrants are frequently under-resourced, stigmatized, and not adequately integrated into primary care. The profound psychological impact of displacement, trauma, and integration challenges often goes unaddressed.
- Vulnerability of Specific Groups: Highly vulnerable groups, such as unaccompanied minors, victims of human trafficking, stateless persons, and undocumented migrants, often fall through the cracks of existing health systems, facing the most extreme forms of exclusion and exploitation.
The Way Forward: Accelerating Progress and Fostering Collaboration
The WHO acknowledges the progress achieved but stresses the urgency for governments, international partners, and donors to accelerate efforts towards comprehensive inclusion. The organization outlines several key areas for action:
- Translate Commitments into Action: Governments must move beyond policy declarations to ensure effective implementation on the ground. This requires clear guidelines, resource allocation, and accountability mechanisms.
- Increase Investment in Inclusive Systems: Sustainable funding for refugee and migrant health must be integrated into national health budgets, reducing reliance on external aid and fostering long-term resilience.
- Strengthen Data Collection and Research: Developing robust data collection systems that disaggregate information by migration status, age, gender, and other relevant factors is crucial for evidence-informed policy and targeted interventions.
- Enhance Health Workforce Capacity: Investing in training and education for healthcare professionals to build cultural competency, language skills, and expertise in migrant health issues is paramount.
- Promote Rights-Based Approaches: Upholding the principle of non-discrimination and ensuring access to health services for all, regardless of legal status, is a fundamental human right and a public health imperative.
- Foster Multi-Sectoral Partnerships: Collaborative efforts between health ministries, immigration authorities, social services, civil society organizations, and international bodies are essential for holistic and effective responses.
- Leverage Digital Health Solutions: Embracing and integrating digital health technologies can improve continuity of care, facilitate access to health information, and streamline administrative processes across borders.
The WHO reiterates its unwavering commitment to supporting Member States in translating these commitments into tangible action. This involves strengthening the evidence base, promoting culturally responsive care models, and facilitating the full integration of refugees and migrants into resilient national health systems. At global, regional, and country levels, the WHO will continue to work closely with key partners, including the International Organization for Migration (IOM), the United Nations High Commissioner for Refugees (UNHCR), and the World Bank, to advance coordinated, rights-based approaches to refugee and migrant health.
Digital Health as a Catalyst for Cross-Border Care
A significant stride in this collaborative effort was marked by the IOM becoming the first international organization to onboard onto the Global Digital Health Certification Network (GDHCN). The GDHCN, a WHO-hosted digital public infrastructure, is designed to enable the secure and verifiable exchange of health documents across national borders. This groundbreaking collaboration is expected to profoundly enhance efforts to assist migrants in securely accessing their verifiable health records wherever they travel, thereby supporting seamless continuity of care across different health systems and national jurisdictions.
By pioneering as the first international organization to join the GDHCN, the IOM not only reinforces its dedication to migrant well-being but also underscores the WHO’s leadership in addressing the critical public health aspects of refugee and migrant health. This initiative signifies a strong commitment to fostering trusted, interoperable digital health systems that protect the health information of individuals and empower people globally, irrespective of their migratory status.
Broader Implications for Global Health and Human Rights
This WHO report and its findings carry profound implications for global health, human rights, and international cooperation. The increasing inclusion of refugees and migrants in national health policies is a vital step towards achieving Universal Health Coverage (UHC) and the Sustainable Development Goals (SDGs), particularly SDG 3, which aims to ensure healthy lives and promote well-being for all at all ages. By systematically addressing the health needs of these populations, countries are not only upholding fundamental human rights but also strengthening their own public health infrastructure against future crises.
The report serves as a powerful reminder that neglecting the health of any segment of society poses risks to the entire population. In an increasingly interconnected world, cross-border health threats necessitate inclusive health systems. The progress documented signals a growing recognition that migrant and refugee health is not a peripheral issue but an integral component of national and global health security. While challenges persist, the emerging trend towards inclusion offers a beacon of hope for a more equitable and healthier future for all. This momentum must be sustained and amplified through continued political will, robust investment, and unwavering commitment to the principle that health is a human right for everyone, everywhere.