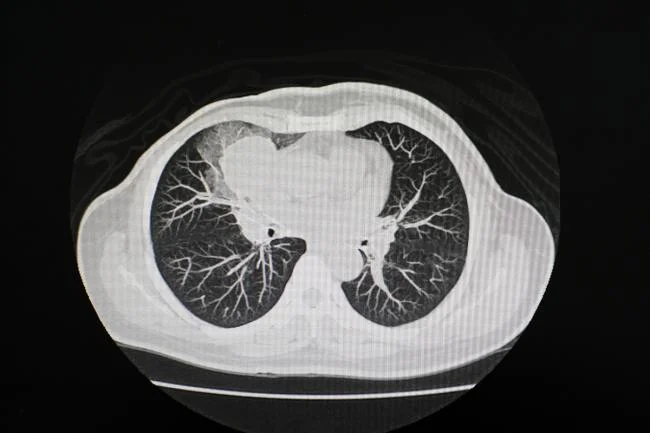
Automated CT scan analysis could fast-track clinical assessments
A groundbreaking research initiative, substantially funded by the National Institutes of Health (NIH), has culminated in the development of a sophisticated machine learning model named Merlin. This innovative artificial intelligence tool is poised to revolutionize medical imaging, offering the potential to significantly streamline diagnoses and unveil critical early markers for chronic diseases years in advance. The team’s findings, published in the prestigious journal Nature on March 4, 2026, detail Merlin’s remarkable versatility and superior performance across a wide array of diagnostic and prognostic tasks.
The core of Merlin’s breakthrough lies in its ability to interpret 3D abdominal computed tomography (CT) scans with unprecedented accuracy and breadth. Unlike previous AI models often purpose-built for specific tasks, Merlin was conceived as a general-purpose CT model. Yet, during rigorous testing, it consistently surpassed the performance of specialized automated tools in tasks these narrower systems were specifically designed to handle. From identifying anatomical features with precision to predicting the onset of complex diseases, Merlin demonstrates a level of adaptability and insight that promises to redefine the landscape of clinical assessment.
The Genesis of Merlin: Leveraging Unprecedented Data
The development of Merlin was predicated on access to a uniquely comprehensive dataset, hailed by researchers as the largest collection of abdominal CT data to date. This invaluable resource was curated from the Stanford University School of Medicine, comprising over 15,000 3D abdominal CT scans meticulously linked to their corresponding radiology reports and nearly one million medical diagnosis codes. This multi-modal training approach, combining visual imagery with rich textual and coded clinical information, allowed Merlin to learn the intricate relationships between what is seen in a scan and what it signifies clinically.
"Rich datasets like this are necessary to push the limits of what artificial intelligence models can accomplish in medicine," stated Bruce Tromberg, Ph.D., director of NIH’s National Institute of Biomedical Imaging and Bioengineering (NIBIB). He further emphasized, "This work exemplifies how meticulously crafted training data can enable remarkable insights that significantly streamline workflows and assist in clinical decision-making." The integration of diverse data types is a hallmark of foundation models, a new class of AI that Merlin exemplifies, trained on large-scale, unlabeled datasets to achieve broad applicability.
Addressing the Growing Strain on Healthcare Systems
The introduction of Merlin comes at a critical juncture for global healthcare, particularly in the United States, where medical imaging plays an increasingly central role in patient care. CT scans are a common diagnostic tool, frequently performed in the early stages of medical evaluations. However, the traditional diagnostic process is often protracted, involving manual interpretation by radiologists, followed by potential additional tests and clinical assessments to confirm a diagnosis. This lengthy workflow is compounded by the escalating shortage of physicians, particularly radiologists, which has placed immense pressure on existing healthcare infrastructure.
According to data from the American College of Radiology (ACR), the demand for medical imaging services has been steadily rising by approximately 4-5% annually, while the growth in the radiologist workforce struggles to keep pace. This disparity leads to increased turnaround times for reports, potential diagnostic delays, and elevated levels of burnout among imaging professionals. The average wait time for a non-urgent radiology appointment can range from days to weeks in many regions, directly impacting patient care pathways and potentially delaying critical interventions.
"With Merlin, you could potentially go beyond traditional radiology and jump straight from imaging to a possible diagnosis. And that’s just one potential use," explained co-first author Louis Blankemeier, Ph.D., who conducted this pivotal work during his graduate studies at Stanford University. This vision suggests a future where AI acts as a sophisticated first-pass interpreter, accelerating the initial stages of clinical assessment and allowing human experts to focus on the most complex or ambiguous cases.
A Gauntlet of Tests: Proving Merlin’s Unrivaled Versatility
To ascertain Merlin’s capabilities, the research team subjected the model to an exhaustive battery of tests across six broad categories of activities, encompassing more than 750 individual tasks. These challenges spanned diagnostics (identifying existing conditions), prognostics (predicting future disease onset), and quality assessment of the scans themselves. The model’s training on a vast trove of clinical data, linking over 15,000 3D abdominal CT scans with their radiology reports and nearly one million diagnostic codes, was instrumental in allowing it to learn the complex relationships between visual and written medical information.
Following its initial training, Merlin was then tasked with interpreting over 50,000 previously unseen abdominal CT scans, sourced from four different hospitals. This crucial step ensured that the model’s performance was not merely a reflection of its training data but demonstrated robust generalizability across varied clinical environments. The goal was to assess how closely Merlin’s automated conclusions could align with the human-produced assessments associated with each scan.
"Merlin tackled some tasks, such as predicting diagnosis codes, head-on, while other more complicated tasks, such as drafting radiology reports from scratch or identifying and outlining organs in a 3D space, called for additional training," noted co-first author Ashwin Kumar, a graduate student at Stanford University. This iterative refinement process highlights the adaptability inherent in foundation models.
In a direct comparison against state-of-the-art models specializing in each task type, Merlin showcased superior or equivalent performance. Across 692 different diagnostic codes, Merlin successfully predicted which of two scans was more likely to be associated with a particular code over 81% of the time, outperforming several variants of two other models. For a critical subset of 102 codes, Merlin’s performance escalated to an impressive 90% accuracy. This level of diagnostic precision suggests that Merlin could serve as a powerful aid in rapidly triaging cases and flagging potential conditions.
Unveiling the Future: Prognostic Power and Biomarker Discovery
Perhaps one of Merlin’s most compelling capabilities lies in its prognostic potential. The team challenged Merlin to predict the onset of chronic diseases—such as diabetes, osteoporosis, and heart disease—in healthy patients, based solely on their CT scans. This endeavor pushes the boundaries of medical imaging beyond immediate diagnosis into the realm of preventive medicine.
The study revealed that when comparing scans from different subjects, Merlin could identify patients at a higher risk of developing a particular disease within the next five years with 75% accuracy, significantly outperforming a competing model which achieved 68%. These findings are particularly profound, hinting that Merlin possesses the ability to detect subtle, key features in scans that may be imperceptible to the human eye. This capability could lead to the identification of novel biomarkers for early disease detection, fundamentally altering how chronic conditions are screened and managed. For instance, detecting early signs of bone density loss indicative of osteoporosis or visceral fat distribution patterns linked to metabolic syndrome could allow for interventions years before clinical symptoms manifest.
Adding to its impressive repertoire, the researchers further challenged Merlin to interpret CT scans of the chest—a body part entirely absent from its initial abdominal CT training material. Demonstrating remarkable cross-domain adaptability, Merlin performed as well as, or even better than, models trained exclusively on chest scans. This generalizable feature recognition capacity is a testament to Merlin’s robust architecture and training methodology, positioning it as a truly versatile diagnostic tool.
The "Magic Touch": Architecture and Training Data
The authors attribute Merlin’s "magic touch" to its innovative architecture and the unparalleled training data. Its design allows it to process complex 3D scans efficiently and build deep, meaningful associations between visual patterns and corresponding written clinical information. This multi-modal learning environment enables the model to understand context and nuance that purely visual or textual models might miss.
Senior author Akshay Chaudhari, Ph.D., a professor of radiology and biomedical data science at Stanford University, expressed high hopes for the model’s future. "Our model and the data will provide the community a robust backbone to build upon," he stated, adding, "From here, the sky’s the limit." The research team anticipates that Merlin’s approach could leverage existing regulatory precedents for simpler tasks, potentially fast-tracking its clinical adoption. Simultaneously, plans are underway to refine Merlin for more intricate challenges, such as generating comprehensive radiology reports from scratch. The researchers also encourage other institutions and users to fine-tune the model with their own specific data, allowing for tailored applications to address unique clinical needs.
Broader Implications and Future Trajectory
Merlin’s advent carries profound implications for the entire healthcare ecosystem.
Impact on Healthcare Efficiency and Patient Outcomes: The immediate benefit is the potential for significantly reduced diagnostic turnaround times. By automating initial assessments, Merlin can help alleviate the workload on radiologists, freeing them to focus on complex cases, interventional procedures, and patient consultations. This efficiency gain translates directly into improved patient flow and potentially shorter wait times for critical diagnoses. For patients, earlier disease detection, particularly for chronic conditions, can lead to personalized and timely interventions, potentially slowing disease progression, improving quality of life, and reducing healthcare costs associated with advanced disease management.
Economic Impact: The optimization of diagnostic processes through AI could yield substantial economic benefits. Reduced need for repeat scans, more accurate initial diagnoses preventing unnecessary follow-up tests, and a more efficient allocation of human resources could lead to significant cost savings for hospitals and healthcare systems. The ability to predict disease onset years in advance also opens avenues for preventive care models, which are generally more cost-effective than reactive treatments.
Workforce Transformation: It is crucial to frame AI tools like Merlin not as replacements for medical professionals but as powerful augmentations. Radiologists’ roles may evolve to include supervising AI systems, validating their outputs, and managing the integration of these tools into clinical workflows. This shift will necessitate new training paradigms for future medical students and continued education for current practitioners, focusing on AI literacy and human-AI collaboration.
Regulatory Pathway and Ethical Considerations: The path to widespread clinical adoption for AI in medicine is complex, requiring rigorous validation and regulatory approval. Bodies like the FDA will need to establish clear guidelines for foundation models that can perform a multitude of tasks. Ethical considerations, such as data privacy, ensuring algorithmic fairness across diverse patient populations, and establishing clear accountability for AI-driven diagnoses, will also be paramount. The researchers’ emphasis on "prior precedent" for simpler tasks and encouraging fine-tuning by users points to a pragmatic approach to navigating these challenges.
Continued Research and Development: Merlin represents a robust foundation. Its open-ended nature invites further research into new applications, potentially extending its capabilities to other body parts, different imaging modalities (e.g., MRI, ultrasound), and even integrating with electronic health records for a more holistic patient view. The collaborative spirit, exemplified by funding from NIBIB, the Medical Imaging and Data Resource Center (MIDRC), the National Heart, Lung, and Blood Institute (NHLBI), and the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), underscores the collective effort required to bring such transformative technologies to fruition.
In conclusion, Merlin is not merely another AI tool; it represents a significant leap forward in the application of artificial intelligence to medical imaging. By leveraging vast, multi-modal datasets and demonstrating unprecedented versatility, diagnostic accuracy, and prognostic capability, it stands poised to redefine clinical assessments, alleviate burdens on healthcare systems, and ultimately, improve patient outcomes across a spectrum of diseases. The journey from discovery to widespread clinical integration will require continued collaboration, careful validation, and thoughtful ethical consideration, but the potential for a healthier future is undeniably brighter with Merlin on the horizon.