The Hypothalamus: A Tiny Brain Structure Orchestrating Aging’s Complex Symphony
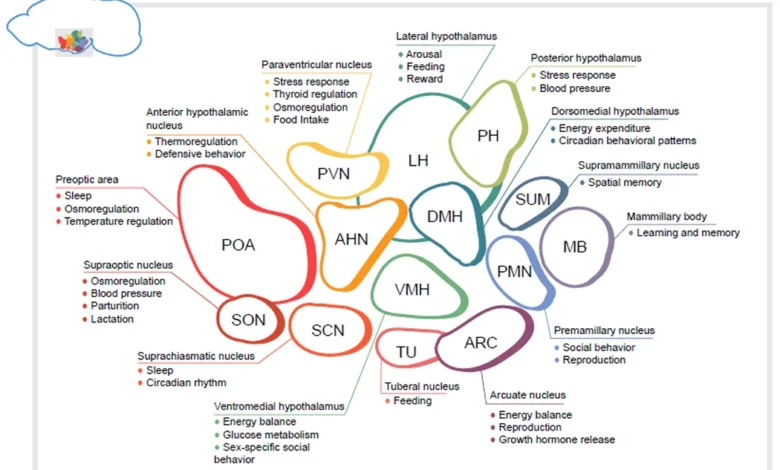
Deep within the intricate architecture of the human brain, nestled above the brain stem and precisely situated between the thalamus and the pituitary gland, lies a structure of profound significance, often underestimated due to its diminutive size. This almond-sized region, known as the hypothalamus, functions as the body’s master regulator, akin to a sophisticated smart home system that meticulously manages temperature, lighting, security, and even the morning coffee brewing. Its primary role is to maintain a delicate internal equilibrium, or homeostasis, by exerting direct influence over the autonomic nervous system. This control is crucial for regulating vital functions such as heart rate, blood pressure, and body temperature. Furthermore, the hypothalamus is a key orchestrator of hormonal signals that govern a vast spectrum of bodily processes, including sleep-wake cycles, mood regulation, appetite, thirst, libido, and even the growth of muscles and bones.
However, as the human body traverses the natural trajectory of aging, the hypothalamus, like many other biological systems, experiences a decline in its finely tuned sensitivity. This diminished responsiveness means it becomes less adept at interpreting and coordinating the complex web of neuronal signals essential for maintaining internal balance. Consequently, a cascade of age-related challenges can emerge, manifesting as sleep disturbances, escalating blood pressure, a noticeable reduction in muscle mass, and unexplained weight gain. The increasing understanding of the hypothalamus’s role suggests that a decline in its function may be a significant, albeit often overlooked, contributor to many of the less desirable physiological changes associated with growing older.
Unraveling the Mysteries of Aging: The Buck Institute’s New Frontier
In its ongoing mission to comprehensively understand the multifaceted process of brain aging, the Buck Institute has recently identified the hypothalamus as a critical new focus area for its research endeavors. Associate Professor Ashley Webb, a leading scientist at the institute, expressed enthusiasm for this burgeoning area of study. "This is the newest focus area in the lab, and it’s always fun to do new things," Webb remarked. "I’m fortunate because people in my lab are really into it." This sentiment underscores the collaborative and driven environment at the Buck Institute as they embark on this complex scientific exploration.
A New Era of Hypothalamic Research Powered by Advanced Technologies
The spearheading of this ambitious project within the Webb lab is credited to postdoctoral fellow Kaitlyn Hajdarovic. Her initial encounter with the hypothalamus occurred during her tenure as a lab technician at Rockefeller University, where she focused on circadian rhythms. Hajdarovic posits that the field of hypothalamic research is currently experiencing a "new golden age," largely propelled by the advent and refinement of single-cell sequencing technologies. She describes the cellular organization within hypothalamic tissue as exceptionally intricate, making it an ideal subject for single-cell analysis. "It has so many different types of neurons that produce so many neuropeptides," Hajdarovic explained. "They all signal to each other, and the neurons respond differently to different cues. Looking at individual cells is the only way to get at what’s happening biologically." This technological leap allows researchers to dissect the hypothalamus’s complexity at an unprecedented level, moving beyond bulk tissue analysis to understand the nuanced behavior of individual cellular components.
Decades of Research Converging on a Central Regulator
The study of the hypothalamus has a long and rich history, with foundational research dating back to the early 20th century. Early work by scientists like Walter Cannon in the 1920s and 1930s laid the groundwork for understanding its role in maintaining a stable internal environment, a concept he termed "homeostasis." Over the subsequent decades, advancements in neuroanatomy, neurochemistry, and molecular biology gradually illuminated the hypothalamus’s diverse functions.
The 1950s and 1960s saw significant progress in identifying specific hypothalamic nuclei and their associated hormones, such as those involved in regulating appetite and metabolism. The discovery of neuropeptides, a diverse class of signaling molecules produced by neurons, further expanded our understanding of the complex communication networks within the hypothalamus. The development of sophisticated imaging techniques and genetic manipulation tools in later decades allowed researchers to probe the hypothalamus’s role in more intricate behaviors and physiological processes.
However, a comprehensive understanding of the hypothalamus’s involvement in aging has remained a relatively nascent area of investigation until more recently. Webb attributes this to the highly specialized nature of previous research. "One of the reasons why people haven’t really looked at aging is because all of these different functions that are regulated by all of these different types of neurons in these little sub-areas of the hypothalamus are studied in individual labs. They really specialize," Webb stated. "The research just hasn’t come together in a way that we felt it needed to in order for us to understand this area of the brain and what that actually means for healthy aging." This fragmentation of research, while leading to deep expertise in specific hypothalamic functions, has historically hindered a holistic view of its role in the aging process. The current research at the Buck Institute represents a deliberate effort to bridge these disciplinary gaps and synthesize existing knowledge into a cohesive understanding of hypothalamic aging.

Modeling Aging in the Lab: From Cell Culture to Animal Studies
Hajdarovic’s current work involves cultivating human hypothalamic neurons in a laboratory setting, a technique known as cell culture. This approach allows for direct observation and manipulation of these crucial cells outside the complex environment of the living brain. Her investigative thought process is driven by fundamental questions: "What factors go into making a hypothalamic neuron? If we can model changes with age, can we screen for drugs that impact the process? Can we take a hypothalamic neuron that looks aged and make it young again?" While acknowledging that these investigations are in their nascent stages, Hajdarovic expressed optimism about the potential of these research questions.
Targeting Appetite and Metabolism: The POMC Neuron Connection
As a primary focus, Hajdarovic is cultivating POMC (pro-opiomelanocortin) neurons. These neurons are strategically located within a specific region of the hypothalamus known as the arcuate nucleus. Their critical role in controlling appetite and maintaining glucose homeostasis is well-established. Studies in animal models have demonstrated that stimulating POMC neurons leads to a reduction in food intake, while diminished activity in these cells is associated with increased food consumption and the development of obesity. "There’s a possibility that these neurons may be related to age-related weight gain," Hajdarovic observed, highlighting a direct link between hypothalamic function and a common challenge of aging. This research holds significant implications for understanding and potentially intervening in age-related metabolic dysregulation.
Investigating Gender Differences and Menopause: A Collaborative Endeavor
The Webb lab is also employing animal models, specifically mice, to further investigate the hypothalamus. This research is being conducted in collaboration with the Kapahi lab, and a deliberate focus on female animals is incorporated due to the pronounced gender differences observed in hypothalamic function. The two labs are pooling their resources and data to compare findings from mice that have undergone ovary removal (a model of hormonal changes experienced by women) with data from naturally aging mice. The overarching goal of this collaborative effort is to elucidate the complex signaling pathways between the hypothalamus and the pituitary gland. This research is expected to provide invaluable insights into the physiological changes that occur in human females during menopause, a significant life transition marked by profound hormonal shifts orchestrated, in part, by the hypothalamus.
Broader Implications for Healthy Aging and Therapeutic Development
The comprehensive research being undertaken at the Buck Institute on the hypothalamus has far-reaching implications for the future of healthy aging. By unraveling the mechanisms by which this crucial brain region declines with age, scientists are paving the way for the development of novel therapeutic interventions. Understanding the specific neuronal populations and molecular pathways involved in hypothalamic aging could lead to targeted treatments for age-related conditions such as obesity, metabolic syndrome, sleep disorders, and mood disturbances.

Furthermore, the insights gained from studying hypothalamic function in the context of aging can inform strategies for promoting longevity and improving the quality of life for an aging global population. As the world’s demographic landscape continues to shift towards an older average age, research focused on preserving and restoring the function of critical regulatory systems like the hypothalamus becomes increasingly vital. The ongoing work at the Buck Institute represents a significant step forward in our quest to not only extend lifespan but also to ensure that those added years are lived in good health and with full cognitive and physical vitality. The intricate symphony of the body, orchestrated by the seemingly small yet mighty hypothalamus, is slowly but surely being deciphered, promising a future where the challenges of aging can be met with greater understanding and more effective solutions.








