I want to know I’m doing absolutely everything I can to preserve my health for as long as possible.
This sentiment echoes across a broad spectrum of society, reflecting a deep-seated human desire not merely to extend life, but to enhance its quality for as long as possible. The vision of maximizing healthspan and lifespan, staving off chronic disease, and retaining vitality well into the ninth, tenth, and even eleventh decades of life is undeniably compelling. However, the path to achieving this often appears fraught with an extraordinary commitment of effort, time, and financial resources, frequently presented with daunting complexity. This article delves into the prevailing narratives surrounding health and longevity, critically examining the efficacy of popular "optimization" strategies against the robust, yet often overlooked, power of fundamental health behaviors.
The Burgeoning Longevity Industry and the Allure of "Optimization"
In recent years, the pursuit of longevity has evolved from a niche scientific interest into a mainstream cultural phenomenon. Podcasts, best-selling books, and social media platforms are awash with advice, often championed by influential figures like Dr. Peter Attia, Dr. Andrew Huberman, Dr. Rhonda Patrick, and biohacker Bryan Johnson. These personalities have brought unprecedented attention to advanced health protocols, promising radical extensions of human healthspan and lifespan through rigorous, data-driven interventions.

The appeal of this content is clear: who wouldn’t want a longer, healthier existence? Furthermore, the structured design and execution of a "perfect" health plan can offer a comforting sense of control in an uncertain world. This movement typically advocates for a multi-faceted approach, encompassing highly specialized diets, extensive supplement regimens, advanced diagnostic testing, personalized exercise programs, and cutting-edge therapies, often referred to as "biohacking." While these approaches promise to unlock unprecedented levels of health, they typically demand a significant investment of both time and capital, raising critical questions about their necessity, accessibility, and ultimate effectiveness.
However, a growing body of evidence, alongside the practical experience of health professionals, suggests that the pursuit of "optimal" might be misguided. For organizations like Precision Nutrition, which has coached hundreds of thousands of individuals with diverse real-life constraints, the concept of "optimal" often proves unrealistic and, more importantly, unnecessary. Their collective experience underscores a pivotal insight: modest, consistent efforts toward fundamental health and well-being frequently yield superior, more sustainable results than intense, highly "optimized" protocols. This perspective challenges the prevailing notion that only extreme measures can lead to exceptional health outcomes, prompting a deeper exploration into the myths and realities of health optimization.
Dispelling the Myths of Hyper-Optimization
The discourse around health and longevity is often clouded by several pervasive myths that can mislead individuals and create unnecessary barriers to genuine well-being.

Myth 1: The "Basics" Are Insufficient for Exceptional Longevity
A common misconception is that achieving significant health improvements and outliving average life expectancies necessitates a battery of complex, "cutting-edge" strategies. This belief often sidelines the foundational elements of health in favor of more exotic interventions.
The Reality: The "basics"—regular exercise, a nutrient-rich diet, adequate sleep, effective stress management, and strong social connections—are profoundly effective. Despite their simplicity, very few individuals consistently adhere to these fundamental practices. According to the Centers for Disease Control and Prevention (CDC), only 24% of American adults meet the recommendations for both aerobic and muscle-strengthening physical activity. Similarly, data from the National Center for Health Statistics indicates that only about 1 in 10 Americans consume the recommended daily servings of fruits and vegetables. The real impediment to widespread longevity and health is not the absence of advanced protocols, but rather the consistent underutilization of these accessible, proven behaviors. If an individual genuinely commits to a well-rounded set of health-promoting actions with 80-90% consistency, they are likely already nearing peak "optimization" in terms of tangible health benefits.
Myth 2: More Effort Always Equates to Better Results
The intuitive appeal of "more is better" often drives individuals to intensify their health regimens, believing that perfectly executed and maximal efforts will guarantee superior health.

The Reality: Health and fitness efforts are subject to the law of diminishing returns. Initial investments in basic health habits yield substantial benefits, but as efforts increase, the incremental gains become progressively smaller. For example, while regular exercise dramatically reduces mortality risk, studies like those on Harvard alumni or large cohorts of older adults show that the steepest declines in risk occur at moderate levels of activity (e.g., 7.5 to 15 MET-hours per week). Beyond this point, further increases in activity continue to reduce risk, but at a continually lower rate. Moreover, excessive engagement in a health regimen can introduce new problems, such as increased risk of injury, burnout, and a reduction in overall life enjoyment. The "Extreme Exercise Hypothesis," for instance, illustrates a U-shaped curve where health risks are highest at very low or extremely high exercise levels, with the lowest risks at moderate to high levels. The goal is not maximal effort, but optimal effort that supports a full, enjoyable life.
Myth 3: Cutting-Edge Strategies Offer Significant, Proven Benefits
Many "longevity optimization" proponents advocate for novel supplements and therapies, implying substantial benefits.
The Reality: Much of the research supporting these advanced strategies is nascent, often conducted on animal models, or involves small-scale, short-duration human observational or theoretical studies. Compounds like resveratrol, NAD+ precursors (e.g., NMN), and various herbal extracts are frequently touted for their anti-aging potential, yet definitive, large-scale human trials demonstrating significant, long-term healthspan or lifespan extension are largely absent. Furthermore, many fringe methods and supplements promoted by influencers lack rigorous scientific validation and can even pose safety risks, especially given the often unregulated nature of the supplement industry. The U.S. Food and Drug Administration (FDA) does not evaluate dietary supplements for safety or effectiveness before they are marketed. Prioritizing foundational, evidence-backed health behaviors is a far more prudent strategy than investing in unproven or potentially unsafe interventions.

Myth 4: Health Is an All-or-Nothing Endeavor
The perceived overwhelming nature of "optimizing" health often leads to inertia, with individuals concluding that if they cannot commit to an extreme regimen, any effort is futile.
The Reality: This "all or nothing" mindset is a significant barrier to health improvement. Data from extensive coaching programs, such as Precision Nutrition’s year-long initiative, consistently show that even clients practicing basic habits less than half of the time achieved measurable and significant results, including weight loss and improved body composition. This demonstrates that consistent, imperfect action is far more effective than striving for an elusive perfection that leads to inaction. Great health is not beyond anyone’s capabilities; it is built on incremental, sustainable changes rather than uncompromising adherence to a rigorous, potentially unsustainable protocol.
The Pillars of Foundational Health: Evidence-Based Behaviors
To genuinely reduce the risk of chronic disease and foster sustained health, the focus should return to a set of fundamental behaviors with robust scientific backing. The challenge lies not in the complexity of these actions, but in their consistent application.

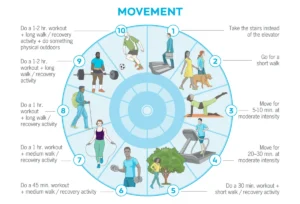
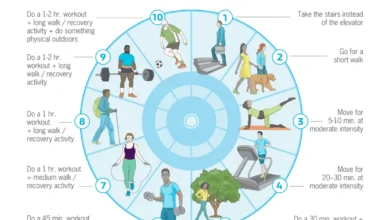
1. Exercise Regularly
Physical activity is universally recognized as a cornerstone of health. Beyond contributing to lean body mass, improved mood, and enhanced energy, exercise is a powerful determinant of longevity. A landmark study of Harvard alumni revealed that any level of physical activity reduced the risk of all-cause mortality, irrespective of body weight, blood pressure, or genetic predisposition. The World Health Organization (WHO) recommends at least 150-300 minutes of moderate-intensity aerobic activity or 75-150 minutes of vigorous-intensity aerobic activity per week, coupled with muscle-strengthening activities on 2 or more days a week.
Optimal Dose: Benefits accrue significantly within these recommended ranges, with diminishing returns for excessive amounts. For example, accumulating 7.5 to 15 MET-hours per week provides the greatest increase in benefits for reducing mortality from cancer, cardiovascular disease, and all causes. While increasing activity beyond this continues to decrease risk, the rate of benefit slows. Furthermore, resistance training is crucial for preserving muscle mass, enhancing cognitive function, improving bone density, and reducing fall risk—a leading cause of death among older adults. Sedentary lifestyles, conversely, are directly linked to increased risks of cardiovascular disease, diabetes, hypertension, and various cancers.
Caveat: While more is generally better up to a point, overtraining can lead to hormonal imbalances, sleep disturbances, chronic fatigue, increased injury risk, and potentially adverse cardiovascular effects in extreme endurance athletes. The goal is consistent, adequate activity, not exhaustive exertion.

2. Eat a Nourishing, Nutrient-Rich Diet
Dietary choices profoundly impact long-term health. Simplicity and consistency are key.
Nutritional Key 1: Prioritize Whole and Minimally Processed Foods: These foods are naturally rich in fiber, healthy fats, vitamins, minerals, and phytochemicals, while being less calorie-dense and containing fewer harmful additives (sugar, sodium, trans fats) than ultra-processed foods (UPFs). Extensive research, including a study involving nearly 10 million participants, has linked UPFs to 32 harmful health outcomes, including type 2 diabetes, mental health disorders, obesity, cardiovascular disease, and all-cause mortality. Aim for 70-80% of your diet to consist of whole or minimally processed foods.
Nutritional Key 2: Consume Five Servings of Fruits and Vegetables Daily: This recommendation, oft-repeated, is backed by substantial evidence. A meta-analysis of over 1.8 million people found that consuming five servings of fruits and vegetables daily was associated with a 13% lower risk of death from any cause, with benefits plateauing at this intake level. The diverse array of phytochemicals in varied colored produce contributes to reduced risks of hypertension, heart disease, stroke, and certain cancers. Currently, only about 10% of Americans meet the five-a-day recommendation.

Nutritional Key 3: Ensure Adequate Protein Intake: Protein is critical for maintaining muscle mass (especially important for preventing sarcopenia and frailty in older adults), supporting bone health, immunity, and satiety. The current USDA recommendation of 0.8 grams per kilogram of body weight is considered a minimum for sedentary individuals. A more robust minimum, particularly for older adults, is 1.2 g/kg (approximately 3-5 palm-sized portions daily), with 1.6-2.2 g/kg being optimal for muscle growth, recovery from vigorous exercise, or for those using GLP-1 medications to mitigate muscle loss. Plant-based proteins are consistently linked to reduced cardiovascular disease risk, while processed red meats should be limited due to their association with increased health risks.
The Role of Supplements: While the market for longevity supplements is booming, their role in genuinely extending health and lifespan is often overstated. Basic supplements like multivitamins or those addressing diagnosed deficiencies (e.g., Vitamin D, iron) can be beneficial. Protein powder can help meet macronutrient needs, and creatine has proven performance benefits. However, many "trendy" longevity supplements (e.g., curcumin, spirulina, NAD+ boosters) lack definitive human efficacy data and can even pose risks, including liver damage. Consulting reputable independent resources like Examine.com and healthcare providers is crucial.
3. Get Adequate Sleep
Sleep is not merely rest; it’s an active and vital physiological process integral to physical and mental health. Research indicates that consistent quality sleep can extend lifespan by several years and is as critical for heart health as diet and exercise. A decrease of just one hour from the ideal 7 hours of sleep per day has been associated with an 11% increased risk of cardiovascular disease and a 9% increased risk of type 2 diabetes. For older adults, adequate sleep (7-8 hours) is crucial for cognitive function, as deep sleep facilitates the clearance of beta-amyloid plaques, implicated in dementia.

Optimal Dose: Sleep experts generally recommend 7 to 9 hours of sleep per night for most adults. While roughly a third of US adults fall short of this, interestingly, consistently sleeping more than 9 hours per night has also been associated with increased health risks, though this may reflect underlying health issues rather than sleep itself being detrimental. The ideal amount of sleep is that which leaves an individual feeling refreshed and energized throughout the day.
4. Manage Stress Effectively
Chronic, unmanaged stress exerts detrimental effects across nearly every physiological system, increasing heart rate, blood pressure, and systemic inflammation, thereby elevating the risk of cardiovascular disease. It also exacerbates mental and emotional health issues, contributing to anxiety, depression, and unhealthy coping mechanisms.
Optimal Approach: Stress is an unavoidable and, in appropriate doses, even beneficial part of life, driving motivation and engagement. The key lies in developing effective coping mechanisms and recovery strategies. These can range from simple mindset shifts (self-compassion, growth mindset) to active self-regulation techniques like deep breathing, journaling, or spending time in nature. The goal is to balance stressors with recovery, viewing stress management as a proportional response to life’s demands. While many report feeling overwhelmed and unsure how to manage stress, even brief, purposeful recovery practices can significantly "refill the tank." Excessive, rigid stress-reduction routines, however, can paradoxically add to stress if they become another chore. The "sweet spot" is feeling energized and engaged, not bored or overwhelmed.

5. Stay Socially Connected
Social connection is a powerful, yet often undervalued, determinant of health and longevity. Strong social and emotional support is linked to improved well-being and a 50% increased likelihood of survival over a given period. The Harvard Study of Adult Development, one of the longest-running studies on human well-being, identified strong relationships as the single greatest predictor of life satisfaction and longevity, surpassing wealth, IQ, or genetics.
Risks of Isolation: Conversely, social isolation and loneliness are profound health risks, comparable to smoking 15 cigarettes a day, and exceeding the risks associated with obesity and physical inactivity. These conditions increase the risk of heart disease, stroke, type 2 diabetes, depression, anxiety, dementia, and premature death.
Optimal Connection: Research suggests that having three to five close friends with whom one interacts regularly (1-3 times per week, in-person or via phone) provides the most significant social benefits. The quality of these connections often outweighs the quantity of acquaintances. While individual needs vary, feeling authentically connected and socially fulfilled is paramount. Excessive social engagement, particularly if it leads to fatigue or involves risky behaviors, can be counterproductive, potentially increasing mortality risk.

6. Minimize Known Harms
Actively avoiding or minimizing exposure to known harmful substances and behaviors is a fundamental aspect of long-term health.
Harm Avoidance 1: Don’t Smoke: Tobacco use remains a leading preventable cause of death globally, responsible for over 8 million premature deaths annually. Smoking is a significant risk factor for coronary heart disease, stroke, emphysema, and numerous cancers, accounting for approximately a quarter of all cancer deaths worldwide. Despite widespread awareness of its dangers, smoking persists as a public health challenge.
Harm Avoidance 2: Limit Alcohol Consumption: The scientific consensus is increasingly clear: alcohol has negative implications for health, particularly with regular, heavy use. Alcohol plays a causal role in over 200 diseases, including liver diseases, heart diseases, at least seven types of cancer, depression, anxiety, and dementia. In 2019, alcohol consumption was linked to 2.6 million deaths globally, and for individuals aged 15-49, it stands as the leading risk factor for death.

Optimal Intake: U.S. guidelines recommend moderate intake: up to one drink per day for women and up to two drinks per day for men. A "drink" is standardized to 14 grams of pure ethanol (e.g., 12 oz beer, 5 oz wine, 1.5 oz spirits). However, recent statements from the WHO emphasize that no amount of alcohol is truly "safe," acknowledging alcohol as a known human carcinogen. While small doses may have minimal impact, risks rise exponentially with heavier drinking (e.g., 4+ drinks on a single occasion for women, 5+ for men, or 8+/week for women, 15+/week for men). The decision rests on an individual’s willingness to tolerate risk relative to perceived benefits, but the healthiest choice for physical health is abstinence or minimal consumption.
7. Practice Basic Preventive Health Measures
Beyond daily habits, consistent engagement in basic preventive healthcare is crucial. This includes regular medical check-ups, appropriate screenings (e.g., blood pressure, cholesterol, cancer screenings), vaccinations, dental care, eye care, and safety practices like wearing seatbelts and helmets. These seemingly mundane actions significantly reduce the risk of serious illness, injury, and premature death. For example, hearing loss, often preventable through ear protection, is the number one modifiable risk factor for dementia. While usage rates for some safety measures like seatbelts are high, adherence to others, such as daily flossing or helmet use among cyclists, remains suboptimal. The objective is reasonable, consistent risk avoidance and health maintenance, not an obsessive elimination of all possible risks.
Bonus: Foster a Sense of Purpose and Meaning
Beyond the physiological, a strong sense of purpose and meaning in life consistently correlates with improved health, overall well-being, and increased longevity. This is distinct from mere happiness and suggests having clear goals and direction. Purpose can manifest in various forms: creative pursuits, career aspirations, community involvement, raising a family, or contributing to a cause. A sense of purpose encourages health-promoting behaviors, improves mental health (reducing depression risk by as much as 43%), and arguably fosters a desire to live longer to fulfill that purpose.

The Trade-offs of Hyper-Optimization: Time, Cost, and Quality of Life
While the foundational health behaviors offer significant, accessible benefits, the path of "hyper-optimization" comes with substantial trade-offs that warrant careful consideration.
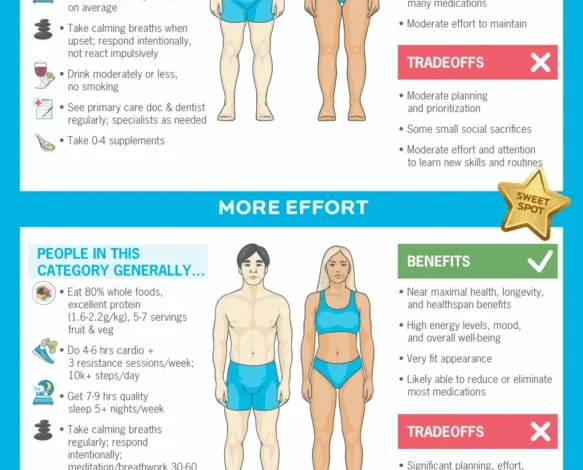
Exorbitant Time and Financial Investment: Comparing a "healthy" individual consistently meeting foundational recommendations with an "optimizer" who pursues maximal efforts and fringe interventions reveals a stark difference in resource allocation. An optimizer might spend three to four times more time and money on health-related activities weekly. This includes extended exercise sessions, intricate meal preparation, elaborate supplement regimens, and advanced recovery techniques (e.g., cryotherapy, red light therapy, hyperbaric oxygen therapy). Beyond weekly routines, optimizers often invest in expensive, less frequent interventions such as comprehensive genetic testing, advanced blood panels, full-body MRI scans, specialized longevity clinics, and bespoke health coaches, easily adding tens of thousands of dollars annually. This immense investment yields increasingly marginal gains, with a "medium-effort healthy" lifestyle likely securing at least 80% of desired lifespan, healthspan, and quality of life improvements.
Impact on Well-being and Quality of Life: The relentless pursuit of "optimization" can paradoxically detract from overall well-being. An excessive focus on physical health can lead to neglect of other crucial aspects of "deep health," including social, emotional, mental, and existential well-being. The rigid adherence to a hyper-optimized protocol can foster social isolation, interfere with enjoyable life experiences (e.g., sharing a meal with loved ones), and induce significant stress if targets are not met. In extreme cases, this preoccupation can manifest as disordered eating (e.g., orthorexia) or other mental health conditions, where the pursuit of health itself becomes a source of anxiety and distress. The essence of a long, healthy life lies not just in extending its duration but in enriching its experience. Enjoying life is not separate from good health; it is an intrinsic component.

Social Determinants of Health: It is also crucial to acknowledge that the capacity to engage in even foundational health behaviors, let alone hyper-optimization, is deeply influenced by social determinants of health. Factors like socioeconomic status, access to quality healthcare, safe environments, education, and freedom from discrimination significantly shape an individual’s health trajectory. For many, the challenges of poverty, racism, lack of accommodation for disabilities, or displacement make consistent adherence to basic health practices exceedingly difficult, if not impossible. This reality underscores the importance of a realistic, compassionate approach: individuals should strive to do the best they can with the resources and circumstances available to them, rather than succumbing to the pressure of an unattainable "optimal."
Conclusion: Making Informed and Intentional Choices
The journey toward a longer, healthier life is deeply personal and requires intentional decision-making.
- Clarify Your Goals: Begin by reflecting on what truly matters most. What kind of life do you envision for yourself, and how does the maximization of healthspan and lifespan align with your broader priorities and values?
- Consider the Trade-offs: Evaluate the practical realities of your life—your time, financial resources, and personal bandwidth. What level of effort are you willing to commit, and what are you prepared to sacrifice (or not sacrifice) to achieve your health goals?
- Prioritize the Basics: Systematically review the foundational health behaviors outlined in this article. Identify areas where you can enhance consistency. For the vast majority of individuals, improving these core habits will deliver tangible, significant, and sustainable results, far outweighing the marginal and often unproven benefits of advanced optimization fads.
- Tune Out the Noise: The constant barrage of information from health gurus and social media can be overwhelming. Remember that you are the ultimate expert on your own life. Make choices that resonate with your personal values and circumstances, rather than blindly following external dictates.
Ultimately, the most effective path to a long and healthy life is one that is sustainable, enjoyable, and integrated seamlessly into a fulfilling existence. It is about making informed choices that prioritize genuine well-being over the relentless, and often unrewarding, pursuit of an elusive "perfection."