Reducing Sodium in Packaged and Prepared Foods Could Prevent Tens of Thousands of Cardiovascular Events in France and the United Kingdom

New research published in Hypertension, a prestigious journal of the American Heart Association, suggests that modest, population-wide reductions in the sodium content of packaged and prepared foods could lead to a dramatic decrease in the incidence of heart attacks, strokes, and premature deaths. By targeting common dietary staples such as bread in France and a wide array of packaged goods and takeaway meals in the United Kingdom, public health officials could achieve significant health improvements without requiring individuals to consciously change their eating habits. These findings underscore the potential of "stealth health" strategies—where food reformulation occurs at the industry level—to mitigate the global burden of cardiovascular disease and reduce the strain on national healthcare systems.
The Physiological Link Between Sodium and Public Health
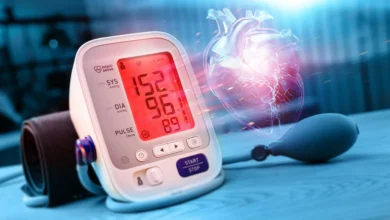
The correlation between excessive sodium consumption and hypertension, or high blood pressure, is well-documented in medical literature. Hypertension remains a primary driver of cardiovascular disease (CVD), which is the leading cause of death globally. When sodium levels in the bloodstream are high, the body retains more water to dilute the salt, increasing the total volume of blood. This extra volume puts added pressure on the walls of the arteries, eventually leading to damage that can cause heart attacks, strokes, chronic kidney disease, and even vascular dementia.
Despite these risks, global sodium intake remains significantly higher than recommended levels. The World Health Organization (WHO) advises that adults consume no more than 2,000 milligrams (mg) of sodium per day, equivalent to roughly 5 grams of salt. The American Heart Association (AHA) sets an even stricter ideal limit of 1,500 mg per day for most adults, particularly those with existing hypertension. However, in many Western nations, average daily intake frequently exceeds 8 to 10 grams of salt, largely due to the prevalence of sodium in processed and restaurant-prepared foods.
The French Case Study: Targeting the National Staple
In France, the strategy to combat hypertension has focused heavily on one of the country’s most iconic and ubiquitous foods: the baguette. In 2019, the French government established a national mandate to reduce overall salt consumption by 30%. Recognizing that bread accounts for approximately 25% of the daily salt intake for the average French citizen, the government entered into a voluntary agreement with the bakery sector in March 2022.
The agreement set a timeline for a progressive reduction in salt levels across all bread products by 2025. Prior to this initiative, traditional French bread contained an average of 1.7 grams of salt per 100 grams. By 2023, the majority of bread producers had already begun meeting the new standards, demonstrating a high level of industry compliance.
To quantify the potential health benefits, researchers led by Dr. Clémence Grave of the French National Public Health Agency utilized mathematical modeling based on national dietary surveys from 2014-2016 and health insurance claims data. The study assumed a scenario of full compliance with the 2025 targets while keeping bread consumption levels constant.
The analysis revealed that meeting these targets would reduce the average daily salt intake by 0.35 grams per person. While this reduction may seem small on an individual basis, the population-level impact is substantial. The model predicted a measurable decrease in systolic blood pressure across the adult population (ages 35 and older), which would translate into thousands of prevented cases of cardio-cerebrovascular disease, kidney failure, and dementia over a single year.
Dr. Grave noted that the "invisible" nature of these changes was key to their success. "This salt-reduction measure went completely unnoticed by the French population—no one realized that bread contained less salt," she stated. This suggests that the human palate can adjust to lower sodium levels if the reduction is gradual, bypassing the resistance often encountered when consumers are asked to change their diets voluntarily.
The United Kingdom: A Comprehensive Approach to Reformulation
While France focused on a specific staple, the United Kingdom has pursued a broader strategy targeting 84 categories of grocery products and 24 categories of "out-of-home" foods, including takeaway meals like pizza, burgers, and curries. The U.K. study, led by Dr. Lauren Bandy of the University of Oxford, examined the potential impact of the country’s 2024 sodium reduction targets.
The U.K. researchers analyzed data from the National Diet and Nutrition Survey (2018-2019), which includes detailed food diaries from a representative sample of the population. They mapped 1,532 unique food items to the government’s sodium reduction categories to estimate how intake would shift if all industry targets were met.
The findings were striking. If the 2024 targets were fully achieved, the average daily salt intake in the U.K. would drop from 6.1 grams to 4.9 grams—a 17.5% reduction. Men, who typically consume more processed and takeaway foods than women, were projected to see even larger decreases in sodium intake and subsequent blood pressure.
Over a 20-year horizon, the model estimated that this reduction would prevent approximately 103,000 cases of ischemic heart disease and 25,000 strokes. Beyond the prevention of acute events, the researchers calculated the impact on "quality-adjusted life years" (QALYs), a metric used to measure the value of health outcomes. The study projected a gain of 243,000 QALYs across the population.
The economic implications are equally significant. The reduction in chronic disease burden was projected to save the National Health Service (NHS) approximately £1 billion (roughly $1.3 billion USD). Dr. Bandy emphasized that while the food industry has made progress, there is still a "lot of room for improvement," particularly in the takeaway and restaurant sectors where sodium levels remain high.
Comparative Analysis: Voluntary vs. Mandatory Strategies
The studies in France and the U.K. highlight two different but complementary approaches to public health policy. The French model relies on a deep dive into a single, high-impact cultural staple, while the U.K. model attempts a broad-spectrum intervention across the entire food supply chain.
Both studies share a common philosophy: removing the burden of change from the consumer. Traditional public health campaigns often focus on education—encouraging people to read labels and choose "low-sodium" options. However, these efforts frequently fail because individual behavior change is difficult to sustain and often limited to higher-socioeconomic groups who have the time and resources to manage their diets.
By contrast, industry-wide reformulation creates a "healthier food environment by default." This approach is more equitable, as it benefits all members of society regardless of their nutritional knowledge or economic status.
Implications for the United States and Global Policy
The results of these European studies have significant relevance for the United States, where approximately 70% of sodium intake comes from processed and restaurant foods rather than the salt shaker at the table. Dr. Daniel W. Jones, a former president of the American Heart Association and chair of the 2025 AHA/ACC High Blood Pressure Guideline, pointed out that the findings validate the "national approach" to sodium limits.
"Though sodium reduction makes small improvements in blood pressure at the individual level, these small changes in individuals result in major improvements in a large population," Dr. Jones explained. In the U.S., the Food and Drug Administration (FDA) has issued voluntary sodium reduction targets for the food industry, but many health advocates argue that more stringent, or even mandatory, standards are needed to replicate the projected successes seen in the U.K. and France.
Methodological Considerations and Limitations
While the findings are promising, the researchers acknowledged certain limitations inherent in modeling studies. For the French study, Dr. Grave noted that it is impossible to isolate the impact of salt reduction in bread from other concurrent factors, such as changes in overall bread consumption or other dietary shifts.
In the U.K., the data relied on self-reported food diaries, which are known to occasionally underestimate actual consumption, particularly for takeaway meals where portion sizes and ingredients can vary. Additionally, the models assume that industry compliance will be 100%, which may not be the case without robust enforcement and monitoring.
Furthermore, these studies focused primarily on systolic blood pressure and its impact on cardiovascular events. They did not fully account for the potential impact of potassium intake, which can counteract some of the negative effects of sodium, or the role of physical activity and other lifestyle factors.
Future Directions: The Role of Industry and Policy
The success of these initiatives depends heavily on the collaboration between policymakers and the food industry. For food companies, the challenge lies in reducing sodium without compromising taste, texture, or shelf life. However, technological advancements in food science—such as the use of sea salt blends, potassium chloride, and flavor enhancers that mimic the "salty" sensation—are making these transitions easier.
The researchers in both countries called for strengthened enforcement of salt reduction policies. In the U.K., there is an ongoing debate about whether voluntary targets are sufficient or if a "salt tax" or mandatory limits should be implemented to ensure laggard companies comply.
As global healthcare costs continue to rise, the argument for preventative measures becomes more compelling. The ability to save billions in healthcare spending while preventing tens of thousands of strokes and heart attacks—all through "invisible" changes to everyday foods—represents one of the most cost-effective opportunities in modern public health.
The studies conclude that if these models are realized, the resulting shift in population health would be profound. By addressing the sodium content in the food supply itself, nations can take a significant step toward "extinguishing" the epidemic of hypertension and its deadly consequences, creating a future where heart health is built into the very fabric of the modern diet.