The Enduring Burden of Healthcare Costs: A Comprehensive Look at American Financial Strain and Health Disparities
The high cost of healthcare remains an overwhelming burden on U.S. families, consistently ranking as the top financial worry for adults and profoundly influencing decisions regarding insurance coverage and care seeking, according to extensive polling data from KFF (Kaiser Family Foundation). This persistent issue, highlighted in KFF’s ongoing Health Tracking Polls and a recent update on April 16, 2026, reveals a healthcare system where financial accessibility is a significant barrier, even for those with insurance. The original KFF brief, first published on December 14, 2021, has been regularly updated to reflect the latest public sentiment and experiences, underscoring the enduring nature of these challenges.
The Pervasive Challenge of Affording Medical Bills
The data paints a stark picture of widespread difficulty in affording medical costs across the United States. Nearly half of all U.S. adults (44%) report that it is either very or somewhat difficult to manage their healthcare expenses. While this struggle disproportionately impacts lower-income households and uninsured individuals, it is by no means exclusive to them. A significant 42% of insured adults still find healthcare costs difficult to afford, illustrating that having coverage does not equate to complete financial protection. Uninsured adults under 65 face an even more dire situation, with a staggering 82% reporting difficulty affording healthcare costs.
Racial and ethnic disparities are also pronounced, with 55% of Hispanic adults and 49% of Black adults expressing difficulty, compared to 39% of White adults. Income level is a strong predictor, as a majority of adults in households earning under $40,000 annually struggle more than those in higher-income brackets. These figures, primarily from the KFF Health Tracking Poll: May 2025, reflect a systemic issue rather than isolated incidents of financial hardship.
Looking specifically at the past year, approximately three in ten adults (28%) indicate that they or a family member experienced problems paying for healthcare. This number surges to four in ten among Hispanic adults (41%) and young adults aged 18 to 29 (40%). Among those under 65, nearly six in ten (59%) uninsured adults reported payment problems, a rate double that of their insured counterparts (30%), as documented in the KFF Health Tracking Poll: November 2025. This recurring pattern underscores that the financial ramifications of medical care are not merely theoretical but are actively impacting millions of American families annually.

Skipping Care: A Dangerous Consequence of High Costs
The financial strain imposed by healthcare costs frequently forces individuals to make difficult choices, often at the expense of their health. One-third (36%) of adults admit to skipping or postponing necessary medical care in the past 12 months due to cost concerns. Women are slightly more likely than men to forgo care (38% vs. 32%). Notably, adults aged 65 and older, largely covered by Medicare, are significantly less likely to delay care due to cost, highlighting the protective role of comprehensive insurance for this demographic.
However, health insurance is not an impenetrable shield. A substantial four in ten insured adults (37%) still report delaying or skipping needed healthcare services because of cost. For uninsured adults, the situation is dire, with three-quarters stating they have foregone care due to financial barriers. These findings, also from the KFF Health Tracking Poll: May 2025, indicate that even with insurance, out-of-pocket expenses, deductibles, and co-pays can be prohibitive.

The ramifications of delayed or skipped care are far-reaching and often detrimental. Nearly one in five adults (18%) report that their health worsened because they could not access or postponed necessary treatment. Among adults under 65, the uninsured are twice as likely as those with coverage (42% vs. 20%) to experience a decline in health due to skipped care. This disparity is even more pronounced when comparing younger adults (23%) to those aged 65 and older (6%), underscoring the vital role Medicare plays in preventing health deterioration linked to cost. A 2022 KFF report further revealed a grim cycle: individuals already burdened by medical or dental debt are disproportionately likely to delay or skip subsequent care, with half (51%) reporting cost as a barrier to recommended tests or treatments (KFF Health Care Debt Survey: Feb.-Mar. 2022).
The High Price of Prescription Drugs
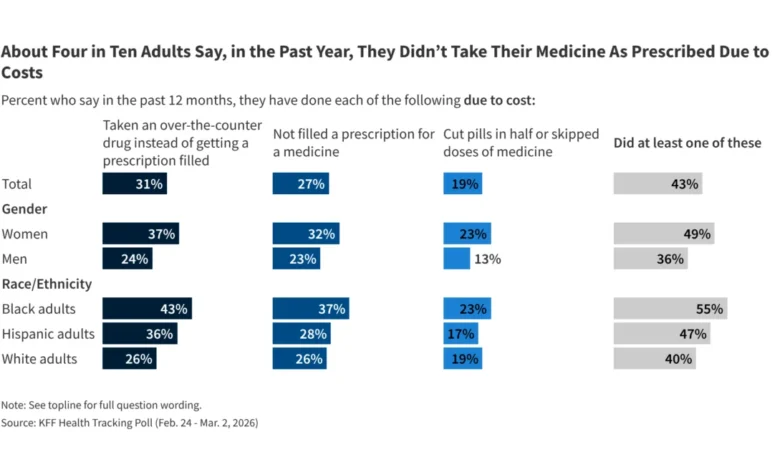
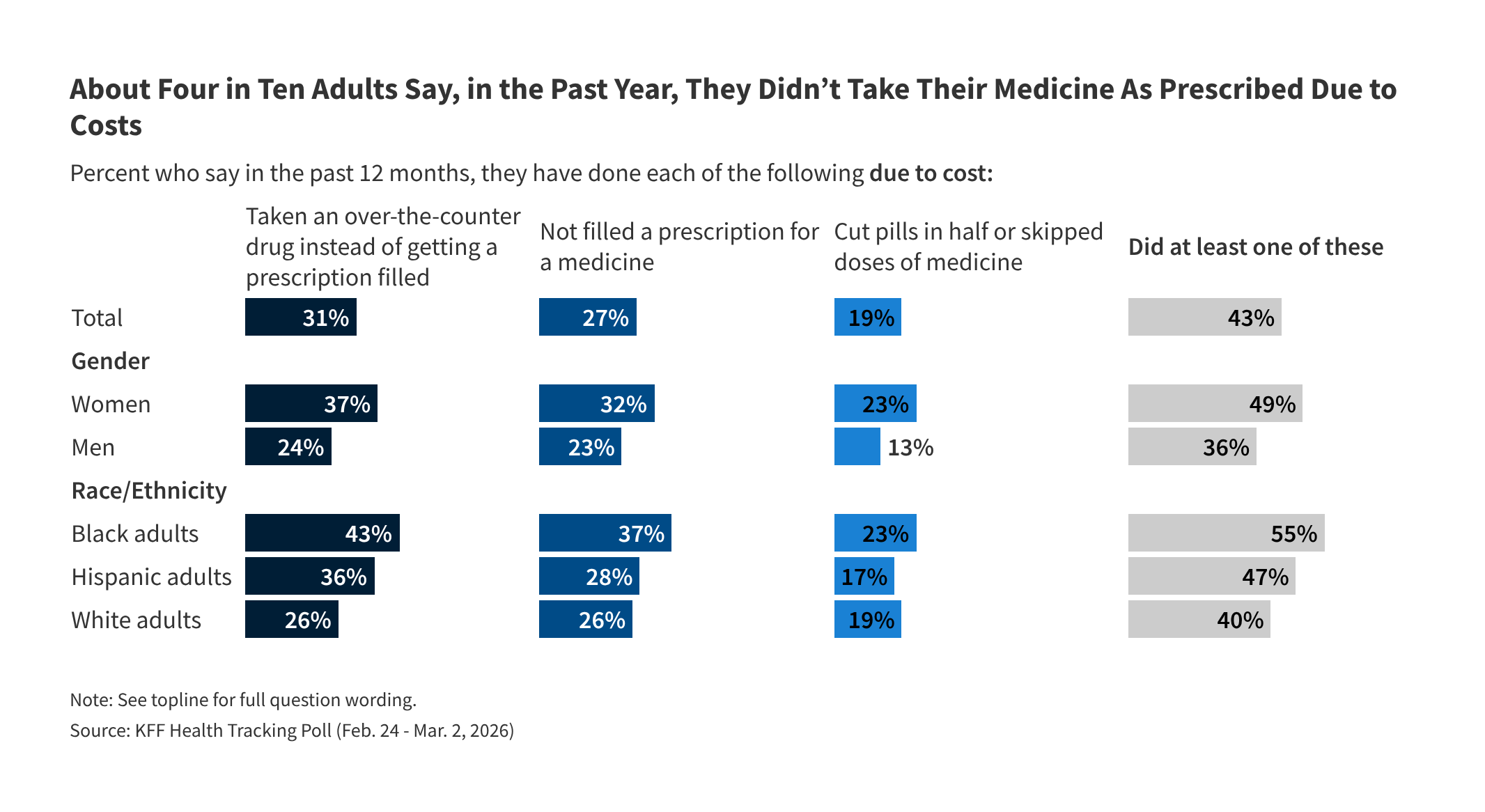
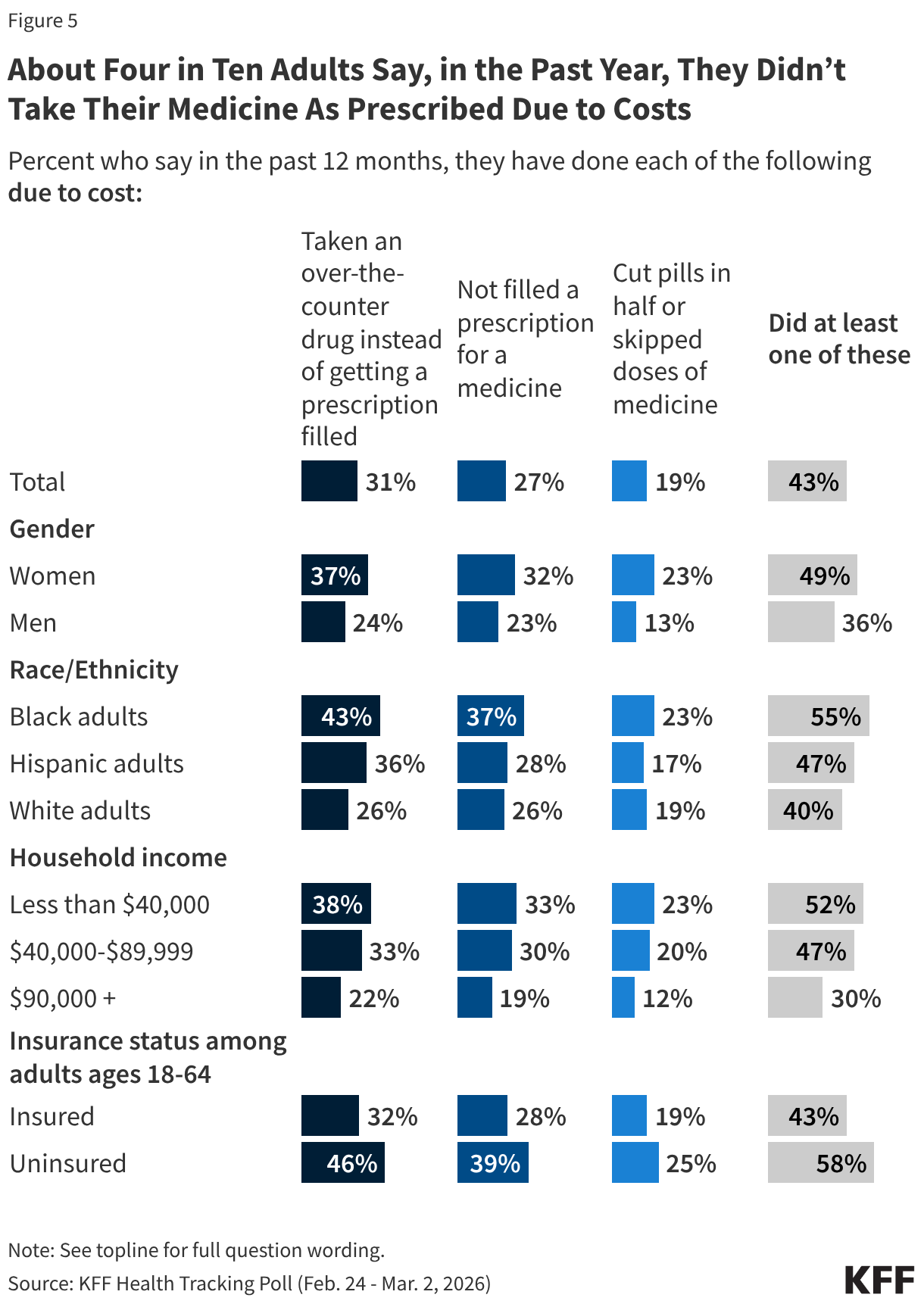
Prescription drug costs represent another critical component of the healthcare affordability crisis. About three in ten adults (31%) have resorted to purchasing over-the-counter medications instead of filling a prescribed drug due to cost concerns in the past year. A quarter (27%) have simply not filled a prescription, and nearly one in five (19%) have taken the dangerous step of cutting pills in half or skipping doses to stretch their supply. Cumulatively, four in ten adults (43%) report taking at least one of these measures in the past year, marking a concerning upward trend from 33% in 2025 and 31% in July 2023.

These cost-saving measures are more prevalent among lower and middle-income households, with about half of adults earning under $90,000 annually resorting to such actions, compared to three in ten adults in higher-income brackets. Uninsured adults under 65 are also more likely to modify their medication use due to cost (58%) than their insured counterparts (43%). Gender and racial disparities persist, with half of women (49%) and over half of Black adults (55%) reporting these measures, compared to 36% of men and 40% of White adults. These statistics, from the KFF Health Tracking Poll: March 2026, highlight the urgent need for solutions to drug affordability, especially as new, expensive specialty drugs become more common.
Health Insurance: A Shield with Cracks
While health insurance is designed to provide financial protection, its own costs—premiums, deductibles, and out-of-pocket expenses—can still create significant burdens. Most insured adults rate their health insurance as "excellent" or "good" for prescription co-pays (61%), doctor visit out-of-pocket costs (53%), and monthly premiums (54%). However, a substantial minority—at least three in ten—rate their insurance as "fair" or "poor" across these metrics.

Affordability ratings vary considerably by insurance type. Adults with private insurance, whether employer-sponsored or Marketplace plans, are more likely to give negative ratings to their monthly premiums, out-of-pocket costs for doctor visits, and prescription co-pays compared to those with Medicare or Medicaid. For instance, about one in four Medicare beneficiaries give negative ratings to their monthly premiums and out-of-pocket prescription costs, and one in five view their doctor visit costs negatively. Medicaid enrollees, benefiting from minimal or no monthly premiums in most states and nominal co-pays, are the least likely to give negative ratings on these affordability measures, underscoring the financial relief offered by such programs. These insights come from the KFF Survey of Consumer Experiences with Health Insurance.
The Shadow of Healthcare Debt
Healthcare debt is a widespread and debilitating problem in the United States. A June 2022 KFF analysis, conducted in conjunction with the investigative journalism project Diagnosis Debt by KFF Health News and NPR, revealed that 41% of U.S. adults carry some form of debt due to medical or dental bills. This includes 24% with past-due or unpaid bills, and 21% who are paying off bills directly to a provider over time. One in six (17%) owe money to banks, collection agencies, or other lenders from loans taken out for medical expenses, while similar shares (17%) have incurred credit card debt for healthcare. A further one in ten report owing money to family or friends for borrowed funds to cover medical bills.
This debt is not evenly distributed. Disproportionate shares of lower-income adults, the uninsured, Black and Hispanic adults, women, and parents are currently saddled with medical or dental debt. The sheer scale of this problem highlights how systemic issues in healthcare financing translate into profound personal financial crises, impacting credit scores, housing stability, and overall economic well-being for millions.
Widespread Vulnerability and Financial Anxiety
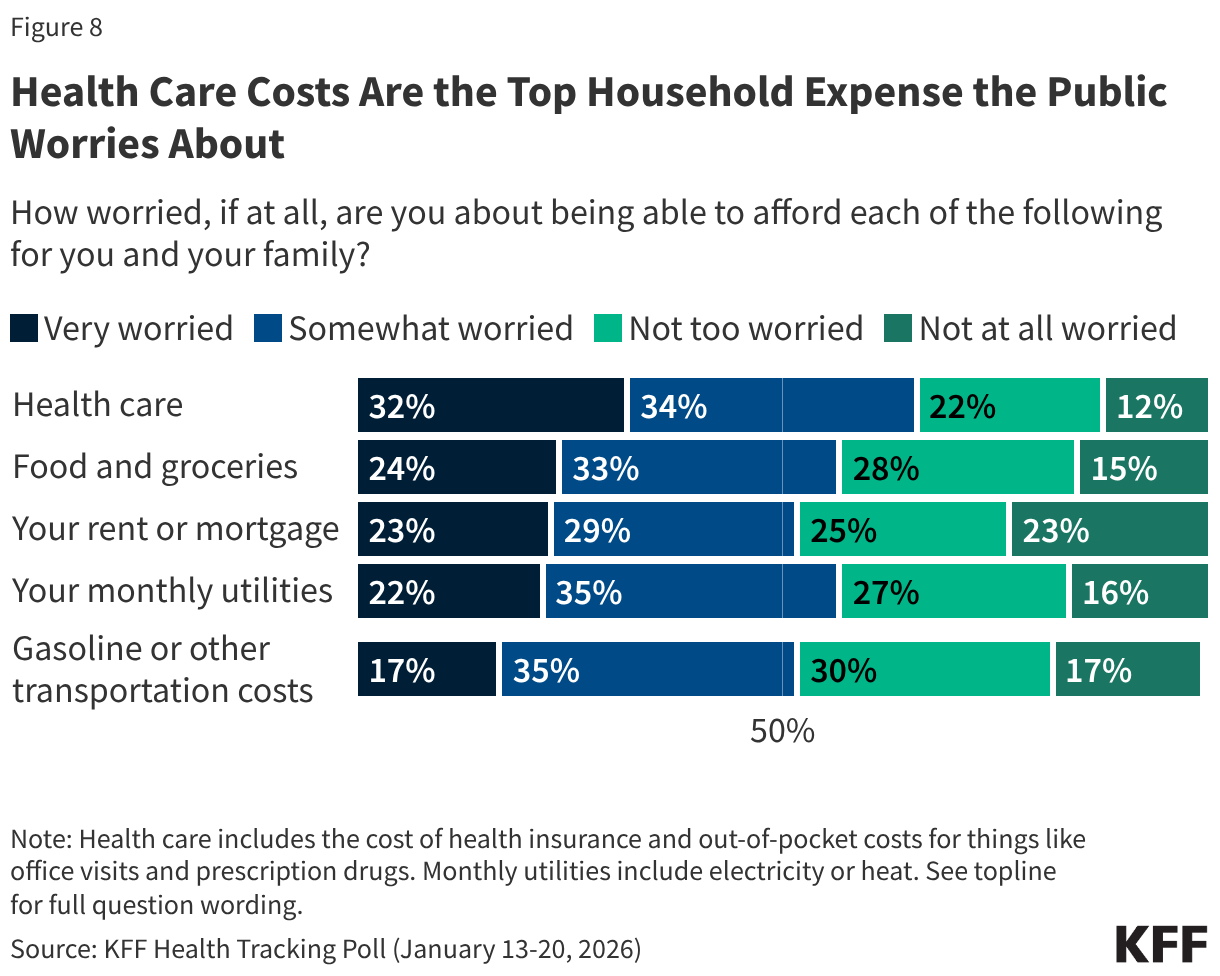
As of early 2026, healthcare costs dominate Americans’ financial worries. Two-thirds (66%) of adults express at least some worry about affording healthcare costs, including insurance premiums and out-of-pocket expenses for visits and prescriptions. This concern surpasses worries about affording food (57%), utilities (57%), housing (52%), and transportation (52%).

This anxiety is particularly acute among the uninsured, with nearly nine in ten (88%) expressing worry about healthcare costs. However, a significant 68% of insured adults also share this concern, demonstrating that the fear of high medical bills transcends insurance status. Healthcare costs consistently rank as the top household financial worry across all insurance types and political affiliations, as per the KFF Health Tracking Poll: January 2026.
The precarious financial position of many Americans is further illustrated by their inability to manage unexpected medical expenses. About half of U.S. adults state they would be unable to pay an unexpected $500 medical bill out of pocket. This includes 19% who couldn’t pay it at all, 5% who would borrow from banks or friends/family, and 21% who would incur credit card debt. Women, lower-income households, Black and Hispanic adults are more likely to face this challenge, highlighting deep-seated economic vulnerabilities that intersect with healthcare access (KFF Health Care Debt Survey: Feb.-Mar. 2022).
Among older adults, the costs of long-term care and support services present another layer of anxiety. Nearly six in ten (57%) adults 65 and older worry about affording nursing home or assisted living facilities, and half are anxious about the cost of paid nurses or aides. These concerns are even more pronounced among those aged 50 to 64, with over seven in ten expressing anxiety about affording residential care (73%) and professional in-home support (72%) if needed. These findings from "The Affordability of Long-Term Care and Support Services: Findings from a KFF Survey" point to a looming crisis for an aging population.

Understanding the Roots of U.S. Healthcare Costs
The persistent and escalating nature of healthcare costs in the U.S. is rooted in a complex interplay of factors unique to the American system. Unlike many other developed nations, the U.S. lacks universal price negotiation for drugs and services, leading to significantly higher prices for everything from prescription medications to hospital procedures. Administrative complexity is another major driver, with a fragmented insurance system and intricate billing processes consuming a substantial portion of healthcare spending. The prevalence of the fee-for-service model incentivizes volume over value, while market consolidation among hospitals and pharmaceutical companies reduces competition, allowing providers and manufacturers to command higher prices. Furthermore, the extensive use of advanced medical technologies and specialized treatments, while beneficial, often comes with a hefty price tag that is not always balanced by efficiency or cost-effectiveness. The original KFF brief, which began tracking these issues in 2021, reflects a period where these systemic challenges have only become more entrenched, culminating in the updated data in 2026 that continues to show a worsening situation for many Americans.
Policy Implications and Calls for Action
The consistent KFF polling data, spanning from its initial publication in 2021 to its latest update in 2026, serves as a powerful call to action for policymakers and healthcare stakeholders. Patient advocacy groups consistently highlight the human toll of these financial burdens, urging for comprehensive reforms. They point to the devastating impact of medical debt on families, the health consequences of skipped care, and the widening health disparities exacerbated by cost barriers.
Policy experts often propose multi-faceted approaches, including enhanced price transparency requirements, allowing Medicare to negotiate drug prices, strengthening the Affordable Care Act (ACA) and expanding Medicaid, and exploring innovative payment models that shift away from fee-for-service. There is also growing interest in medical debt relief initiatives and consumer protections against surprise billing. While healthcare industry representatives often emphasize the costs of research and development, regulatory compliance, and maintaining a high standard of care, the public outcry and empirical data from KFF suggest that the current system is unsustainable for many. The continuity of KFF’s polling over these years underscores that despite ongoing policy debates and incremental changes, the fundamental problem of healthcare affordability in the U.S. remains largely unresolved, demanding renewed urgency and bolder solutions to safeguard the financial and physical well-being of its citizens.
Conclusion

The latest KFF polling data, updated in April 2026, unequivocally demonstrates that high healthcare costs continue to inflict severe financial hardship on American families. From difficulties affording basic medical care and prescription drugs to the accumulation of debilitating debt and widespread financial anxiety, the current system is failing a significant portion of the population. The persistent nature of these challenges, consistently tracked since 2021, highlights an urgent and systemic problem that demands comprehensive and equitable solutions. Without meaningful reforms, millions of Americans will continue to face agonizing choices between their health and their financial stability, perpetuating a cycle of debt, delayed care, and worsened health outcomes.