Scientists discover why some wounds refuse to heal
An international research team led by Nanyang Technological University, Singapore (NTU Singapore) has identified a groundbreaking pathway to accelerate the healing of chronic wounds, offering a new strategy to combat infections even when they are caused by highly antibiotic-resistant bacteria. The study, published in the prestigious journal Science Advances, represents a significant shift in medical science, moving away from the traditional focus on eradicating bacteria and toward neutralizing the specific metabolic processes that prevent human tissue from repairing itself.
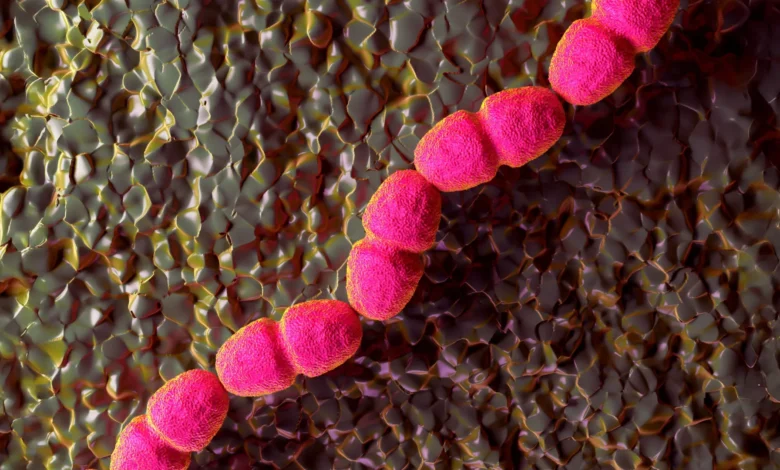
The research was a collaborative effort involving experts from the University of Geneva, Switzerland, and the Singapore Centre for Environmental Life Sciences and Engineering (SCELSE). By uncovering the precise biological mechanism by which the bacterium Enterococcus faecalis (E. faecalis) stalls the healing process, the team has opened the door to a new generation of treatments that could prevent thousands of amputations globally each year.
The Growing Global Crisis of Non-Healing Chronic Wounds
Chronic wounds, defined as wounds that fail to proceed through an orderly and timely series of events to produce anatomical and functional integrity, have become a silent epidemic. These injuries include diabetic foot ulcers, pressure sores, and venous leg ulcers. Globally, the statistics are staggering: approximately 18.6 million people develop diabetic foot ulcers every year. For individuals living with diabetes, the lifetime risk of developing a foot ulcer is as high as one in three.
The consequences of these wounds are often devastating. Chronic wounds are the primary precursor to lower-limb amputations, as persistent infections can lead to gangrene or systemic sepsis. In Singapore, the problem is particularly acute due to an aging population and high rates of diabetes. Local data indicates that more than 16,000 cases of chronic wounds are reported annually, with a disproportionate impact on older adults.
The financial burden on healthcare systems is equally immense. Treating chronic wounds requires frequent dressing changes, long-term antibiotic use, and often surgery. When these wounds fail to heal, the cycle of hospital readmissions creates a massive drain on resources and significantly reduces the quality of life for patients and their caregivers.
Unmasking the Culprit: How E. faecalis Sabotages Recovery
For decades, the medical community has recognized that the presence of certain bacteria correlates with poor wound healing. However, the specific "how" remained elusive. The NTU-led study focused on Enterococcus faecalis, an opportunistic pathogen commonly found in the human gut that frequently migrates to wound sites.
Unlike many other pathogens that rely on lethal toxins to destroy host tissue, E. faecalis employs a more subtle and insidious strategy. The research team, led by NTU Associate Professor Guillaume Thibault and Professor Kimberly Kline of the University of Geneva, discovered that E. faecalis utilizes a metabolic process known as extracellular electron transport (EET).
Dr. Aaron Tan, an NTU Research Fellow and the study’s first author, found that through the EET process, the bacteria continuously release reactive oxygen species (ROS), specifically hydrogen peroxide. While the human body uses small amounts of hydrogen peroxide for signaling, the concentrated and sustained release from E. faecalis creates a toxic environment for surrounding skin cells.
The Science of Cellular Paralysis: ROS and the Unfolded Protein Response
The core of the discovery lies in how these bacterial byproducts affect keratinocytes—the primary cells in the epidermis responsible for closing a wound. Under normal circumstances, when the skin is broken, keratinocytes migrate from the edges of the wound to the center, creating a new barrier.
The study revealed that the hydrogen peroxide produced by E. faecalis triggers a "stress alarm" within the keratinocytes known as the unfolded protein response (UPR). The UPR is a natural defense mechanism intended to help a cell survive temporary damage by pausing the production of new proteins and focusing on repairing existing ones.
However, in the presence of a persistent E. faecalis infection, the UPR is kept in a state of constant activation. This chronic stress effectively paralyzes the keratinocytes. Instead of migrating to seal the wound, the cells remain stationary and focused on internal survival. This cellular "lockdown" is the primary reason why many infected wounds remain open for months or even years.
To verify this finding, the researchers engineered a mutant strain of E. faecalis that lacked the genetic ability to perform extracellular electron transport. When this modified bacterium was introduced to skin cells, hydrogen peroxide levels remained low, and the keratinocytes were able to migrate and heal the wound normally. This confirmed that the bacteria’s metabolism, rather than its mere presence or its toxins, was the weapon blocking recovery.
A Paradigm Shift: Neutralizing Metabolism Over Killing Bacteria
One of the most significant implications of this research is its potential to bypass the problem of antimicrobial resistance (AMR). Many strains of E. faecalis have already evolved to resist vancomycin and other "last-resort" antibiotics, making traditional treatments increasingly ineffective.
The NTU team proposed a different approach: rather than trying to kill the bacteria, doctors could simply neutralize the harmful substances they produce. In laboratory experiments, the researchers treated the infected, stressed skin cells with catalase, a naturally occurring antioxidant enzyme that breaks down hydrogen peroxide into water and oxygen.
The results were remarkable. Once the catalase neutralized the hydrogen peroxide, the oxidative stress on the keratinocytes vanished. The "unfolded protein response" deactivated, and the cells regained their ability to move and heal the wound.
"Our findings show that the bacteria’s metabolism itself is the weapon, which was a surprise finding previously unknown to scientists," explained Associate Professor Guillaume Thibault. "Instead of focusing on killing the bacteria with antibiotics, which is becoming increasingly difficult and leads to future antibiotic resistance, we can now neutralize it by blocking the harmful products it generates. We are targeting the actual cause of the chronic wound—the reactive oxygen species—rather than just the source."
Chronology of the Research and Future Clinical Path
The journey to this discovery involved several years of interdisciplinary work. The timeline of the research highlights the meticulous nature of the study:
- Initial Observation: The team began by analyzing the microbial landscape of chronic wounds, noting the prevalence of E. faecalis in non-healing ulcers.
- Metabolic Mapping: Using advanced biochemical assays, the researchers identified the extracellular electron transport (EET) pathway in E. faecalis as a high-activity process during infection.
- Cellular Interaction Studies: The team conducted co-culture experiments, placing E. faecalis in contact with human keratinocytes to observe the real-time impact on cell migration.
- Genetic Validation: The creation of "knockout" bacterial strains proved that the EET pathway was the specific driver of healing inhibition.
- Antioxidant Testing: The final phase involved using catalase and other antioxidants to successfully reverse the cellular paralysis.
Looking forward, the research team is moving toward human clinical trials. The next step involves identifying the most effective delivery systems for these antioxidants. One promising avenue is the development of advanced wound dressings—such as hydrogels or specialized bandages—infused with catalase or similar antioxidant compounds. These dressings would provide a sustained release of the neutralizing enzyme directly to the wound bed.
Broader Implications for Healthcare and Industry
The implications of this study extend far beyond E. faecalis. The discovery that bacterial metabolism can manipulate human cell signaling pathways suggests that similar mechanisms may be at play in other types of chronic infections, such as those found in the lungs or the urinary tract.
Furthermore, because antioxidants like catalase are already widely used in various industries and are well-understood by regulatory bodies, the path to clinical approval could be significantly shorter than that for a new class of antibiotics. This is a critical advantage in the race against rapidly evolving "superbugs."
Medical professionals have reacted with cautious optimism. If the results from the human skin cell models translate successfully to human patients, it could fundamentally change the standard of care for diabetic patients. Instead of months of painful treatments and the constant threat of amputation, patients might see their wounds close in a fraction of the time using topical antioxidant therapies.
By shifting the battlefield from the destruction of the pathogen to the protection of the host cell, the NTU Singapore team has provided a new blueprint for 21st-century medicine. In the ongoing fight against antibiotic resistance, this discovery serves as a reminder that understanding the subtle dialogue between bacteria and human cells is the key to unlocking the body’s innate power to heal.